Doctor-child communication and caregivers’ willingness to recommend hospital: a secondary analysis using pediatric patient experience data
Highlight box
Key findings
• Encouraging the child to ask questions was significantly associated with overall hospital ratings and willingness to recommend the hospital. The child’s perceived health status was a significant covariate for overall hospital ratings. Path analysis revealed that the overall hospital rating partially mediated the relationship between encouraging questions and recommendation willingness, accounting for 57.81% of the total association.
What is known and what is new?
• Effective doctor-child communication is crucial for pediatric care quality and caregiver satisfaction but is often studied as a broad construct.
• This study deconstructs communication into specific behaviors, revealing that encouraging child questions is a distinct, powerful driver of caregiver loyalty (willingness to recommend), operating both directly and indirectly through the overall hospital evaluation.
What is the implication, and what should change now?
• Empowering children to participate in medical dialogues is a critical, high-yield component of patient-centered care that significantly shapes family trust and advocacy.
• Pediatric communication training should prioritize techniques to actively solicit and address children’s questions. Healthcare institutions must support this with systemic measures, such as protecting adequate consultation time and integrating roles dedicated to facilitating child-friendly communication.
Introduction
Background
Hospitalization poses distinct biopsychosocial challenges for pediatric patients. Their immature cognitive and emotional development increases vulnerability to medical trauma: unlike adults, children often lack words to describe symptoms and may see routine procedures as threats, causing heightened anxiety and resistance (1,2). These vulnerabilities are further compounded by the triadic structure of pediatric care, conceptualized as a “Patient Duality” framework (3). Physicians must balance children’s limited understanding, caregivers’ information needs, and the dynamic interaction between them, creating unique communication complexity. In this context, effective communication extends beyond information transmission and becomes a cyclical process of building therapeutic alliance and mutual trust (4). Notably, caregivers function as observers whose evaluations are influenced not only by clinical outcomes but also by the quality of physicians’ engagement with the child. This phenomenon, described as proxy-perceived quality, suggests that caregivers assess healthcare quality through their interpretations of clinician-child interactions (5,6). The Child Hospital Consumer Assessment of Healthcare Providers and Systems (Child HCAHPS) (7) addresses the challenge of quantifying pediatric care experiences. Among its measures, a dedicated domain assesses doctor-child communication via three behaviors—listening, explaining, and encouraging questions—which directly correspond to the fulfillment of a child’s basic psychological needs for relatedness, competence, and autonomy, as proposed by Self-Determination Theory (SDT) (8,9). From an SDT perspective, communication that supports these needs reduces anxiety, enhances perceived control, and fosters trust, thereby improving the subjective experience of care.
To further clarify how such communication behaviors translate into caregivers’ evaluations and behavioral intentions, this study incorporates the Cognitive-Affective-Conative (CAC) framework. The CAC model conceptualizes attitude formation as a sequential process in which external stimuli shape cognitive appraisals, which elicit affective responses and ultimately guide conative intentions (10). Applied to pediatric inpatient care, doctor-child communication serves as the initial stimulus influencing caregivers’ cognitive judgments about care quality and professionalism. These cognitive appraisals subsequently generate affective reactions, such as reassurance, trust, and satisfaction, which are reflected in overall hospital ratings. Finally, these affective evaluations inform conative outcomes, particularly caregivers’ willingness to recommend the hospital to others. Integrating SDT with the CAC framework thus provides a multi-level explanatory structure: communication behaviors satisfy children’s psychological needs, shape caregivers’ cognitive and emotional evaluations, and ultimately influence recommendation intentions.
Rationale and knowledge gap
Prior research on hospitalized children’s doctor-patient communication focuses on three areas: communication’s role in reducing treatment pain (11) and boosting adherence (12); barriers like jargon overuse, caregiver anxiety, and time constraints (13); and triadic (physician-parent-child) shared decision-making (3,14). Yet several critical gaps remain. First, while triadic communication is conceptually prioritized, evidence regarding its practical implementation remains limited, particularly in navigating the patient duality where clinicians must simultaneously engage both the child and caregiver (3). Second, studies often marginalize physician-child interactions—despite their impact on caregiver trust (15)—and fail to disaggregate which discrete behaviors drive stakeholder perceptions (16). Furthermore, the psychological mechanism of proxy-perceived quality (6), where caregivers’ evaluations are shaped by observing clinician-child engagement, requires further empirical exploration within systemic metrics like HCAHPS (17).
While Child HCAHPS has guided pediatric communication research (18), inconsistencies persist regarding its link to caregivers’ global hospital ratings. Only a weak connection exists between communication quality and overall care scores in some contexts (19), whereas communication emerges as a strong predictor of caregivers’ willingness to recommend a hospital (20). These conflicts stem from unaddressed confounders (21), incomplete case-mix adjustments (22), and treating communication as a single construct rather than a multi-dimensional one (23). By identifying these specific associations, this study seeks to provide preliminary evidence and practical clues for prioritizing communication targets in high-pressure clinical settings, shifting pediatric quality improvement from general compliance to evidence-based behavioral strategies.
Objective
This study aims to clarify how three specific doctor-child communication behaviors influence caregivers’ overall hospital rating and willingness to recommend, thereby identifying evidence-based priorities for improving pediatric care quality. We present this article in accordance with the STROBE reporting checklist (available at https://tp.amegroups.com/article/view/10.21037/tp-2025-1-887/rc).
Methods
Study design and setting
This study was a secondary analysis of a cross-sectional, multicenter patient experience survey conducted across six China National Regional Center for Pediatric (NRCP) hospitals. These centers represent the highest-level specialized pediatric hospitals in China and cover six major geographic regions (Northeast, North, East, Central South, Southwest, and Northwest). Caregiver-completed survey data were collected during the first quarter of 2021 using a validated Chinese version of the Child HCAHPS (24). The Chinese version adapted selected items—such as the child’s ethnicity, respondent education level, and preferred language—to ensure cultural appropriateness within the Chinese context. The survey assessed child and family characteristics, caregivers’ perceptions of doctor-child communication, and overall hospital ratings (22,25).
Data collection was conducted on the day of discharge. During the study period, a survey Quick Response (QR) code was displayed in the inpatient ward nurse station area of each participating hospital. Trained research assistants invited eligible caregivers to complete the questionnaire using a smartphone-based online survey platform. Respondents accessed the survey via their own mobile device or a device provided by the research assistant. For caregivers without smartphone access, a paper-based questionnaire was provided.
All research assistants received standardized training on eligibility assessment, proxy reporting procedures, and data collection protocols. Participating hospitals’ nursing departments provided logistical support but were not involved in data analysis.
The online survey system incorporated predefined real-time validation rules, including logic and completeness checks, to enhance data quality and ensure data integrity at the point of entry.
The study was conducted in accordance with the Declaration of Helsinki and its subsequent amendments. The ethical approval was obtained from the Ethics Committee of the Institute of Medical Information, Chinese Academy of Medical Sciences and Peking Union Medical College (No. IMICAMS/04/19/HREC) and individual consent for this retrospective analysis was waived.
Study participants
Recruitment was conducted over a three-month period of pediatric inpatient discharges at each participating hospital. This study adopted a census approach within the predefined recruitment period. All eligible pediatric patients discharged during the study period were invited to participate. No probabilistic sampling design or sampling fraction was applied. Participation was voluntary; caregivers who declined participation or were unable to complete the questionnaire were not included.
Eligibility criteria were consistent with Agency for Healthcare Research and Quality (AHRQ) Child HCAHPS protocols. Inclusion criteria were: (I) children aged ≤17 years and their parents/guardians; (II) at least one overnight hospital stay; and (III) survival to discharge. Exclusion criteria were: (I) discharge against medical advice; (II) discharge to hospice care; (III) absence of a parent/guardian; (IV) a psychiatric principal diagnosis; and (V) admission for observation only.
For the present analysis, we included children aged 3–17 years who were able to communicate with healthcare professionals regarding their health conditions. Questionnaires with incomplete key demographic information were excluded from the final analysis (22,25).
To ensure adequate hospital-level reliability for cross-hospital comparisons, we aimed to obtain at least 300 completed questionnaires per hospital in accordance with AHRQ recommendations. Although all eligible patients during the study period were invited to participate, an a priori sample size calculation was conducted to ensure adequate statistical power for the planned path analysis. For the initial multiple regression model, assuming a small effect size (f2=0.02), a statistical power of 0.80, a significance level of α=0.05, and nine predictors, the minimum required sample size was estimated to be 788. The final analytic sample exceeded the minimum required sample size and ensured adequate statistical power for the mediation analysis (26).
Variables
Sociodemographic characteristics
We collected information on child patient characteristics include: age (categorized as 3–6, 7–9, 10–12, and 13–17 years), gender (male/female), and global health status (rated by caregivers as “Poor or fair”, “Good”, “Very Good” or “Excellent”). As well as the family caregiver characteristics recorded in the survey: age (categorized as <25, 25–34, 35–44, ≥45 years), education level (categorized as “Primary school or less”, “Junior high school”, “High school graduate”, “Some college or 2-year degree”, “4-year college graduate”, “More than 4-year college degree”), and relationship to the child (father, mother, grandparents, other).
Doctor-child communication
Caregivers’ perceptions of doctor-child communication were assessed using three items from the Child HCAHPS, reflecting pediatric-specific interaction quality:
- Doctors listen carefully to the child (henceforth, “listen carefully to child”);
- Doctors explain things in a way that is easy for the child to understand (henceforth, “easy for child to understand”);
- Doctors encourage the child to ask questions (henceforth, “encourage child to ask questions”).
Each item was scored on a 4-point Likert scale (1= “Never” to 4= “Always”), with higher scores indicating better communication. A composite score for doctor-child communication was calculated as the average of the three items to reflect overall communication quality.
Caregivers’ global ratings of hospitals
Two single-item global rating measures were used to assess the quality of pediatric care:
- Overall rating of the hospital;
- Recommend hospital to family and friends (henceforth, “willingness to recommend the hospital”).
Caregivers of patients are asked to rate the hospital on a scale of 0 to 10, with 0 being the worst and 10 being the best, and reported their likelihood of recommending the hospital to other families on a 4-point Likert scale (1= “Definitely no” to 4= “Definitely yes”), with higher scores indicating stronger recommendation intent.
Statistical analysis
All analyses were performed with the statistical software package R (http://www.R-project.org, version 4.4.2; The R Foundation) and EmpowerStats (http://www.empowerstats.com, X&Y Solutions, Inc., Boston, MA). Individuals with missing data are excluded.
In terms of descriptive statistics, frequencies and percentages (%) were used to summarize categorical variables of child and family caregiver’s characteristics, while mean and standard deviation (SD) were used for continuous variables. Hospital-level top-box scores for doctor-child communication and global ratings were calculated and presented by NRCP region, to enable cross-hospital comparison. Additionally, “Top-Box scores” were computed for each communication item and the composite score at the hospital level.
All outcome variables (i.e., overall hospital rating, willingness to recommend the hospital) were recoded into three ordinal categories (Bottom box, Middle box, and Top box) in accordance with CAHPS reporting guidelines. For the 4-point willingness-to-recommend item, Definitely no and Probably no (corresponding to “Somewhat no” in CAHPS terminology) were categorized as Bottom box, Probably yes (“Somewhat yes”) as Middle box, and Definitely yes as Top box. For the 0–10 overall hospital rating scale, scores of 0–6 were classified as Bottom box, 7–8 as Middle box, and 9–10 as Top box.
Association analysis by ordinal logistic regression models were conducted to examine the associations between doctor-child communication (independent variables: x1 x2 x3, three communication items) and caregivers’ evaluations (dependent variables: y1 overall hospital rating, y2 willingness to recommend the hospital). Two models were run for each outcome:
- Model 1: unadjusted (only independent variables included);
- Model 2: adjusted for covariates (child global health status, caregiver age, caregiver education level, caregiver relationship to the child)—covariates were selected based on their potential to confound the relationship between communication and ratings, as identified in prior Child HCAHPS studies (24).
All statistical tests were two-sided, and P<0.05 were considered to indicate statistical significance. Results are presented with 95% confidence intervals (CIs). The strength of associations was reported using regression coefficients (β), and the explanatory power of each model was evaluated using the McFadden R2.
An exploratory path analysis model was employed to examine whether overall hospital rating was statistically associated with the relationship between doctors encourage the child to ask questions (independent variable) and willingness to recommend the hospital (dependent variable). Because all variables were measured simultaneously using cross-sectional data, temporal precedence cannot be established; therefore, the model does not support causal mediation inference. Instead, the analysis evaluates the pattern of associations among variables consistent with a hypothesized mediation structure. Path coefficients corresponding to the direct and indirect associations were estimated, and statistical significance was assessed using 95% CIs. The proportion of the total association accounted for by the indirect pathway was calculated to describe the relative strength of the indirect association, rather than to imply a causal mediation effect. Given the cross-sectional design, the mediation analysis was conducted as an exploratory examination of statistical associations rather than as a test of causal mechanisms. Post-hoc power analyses indicated that the final sample size provided adequate statistical power for both the logistic regression and path analysis models. Internal consistency reliability of the three doctor-child communication items was assessed using Cronbach’s α coefficient in the present sample.
Path analysis was performed using the lavaan package (version 0.6-17). Model fit was assessed using comparative fit index (CFI), Tucker-Lewis index (TLI), root mean square error of approximation (RMSEA), and standardized root mean square residual (SRMR) (27,28).
Results
Characteristics of child patient and family respondent
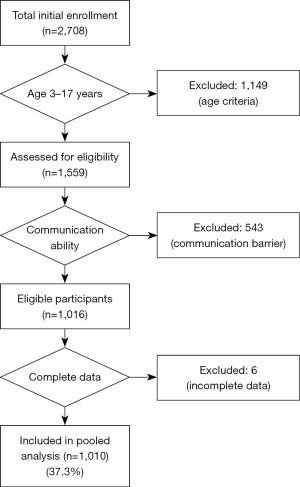
As presented in Figure 1, a total of 2,708 questionnaires were distributed across six regional centers. Of these, 1,559 were returned and met the age eligibility criterion (3–17 years), yielding a recovery rate of 57.57%. After screening for communication capacity and response validity, 1,016 questionnaires were considered effective (65.17% of recovered questionnaires). Following data completeness and logical consistency checks, 1,010 questionnaires were included in the final analysis, corresponding to a final valid response rate of 37.30%. The data completeness rate among effective respondents was 99.41%. Among the pediatric patients, 85.0% were under 12 years of age, and 59.2% were male. A majority of respondents rated their child’s health status as either very good (36.9%) or excellent (49.6%). The family respondents consisted predominantly of mothers (68.5%), with more than half (52.2%) aged 35–44 years. Additionally, 34.1% of the respondents had attained a college-level education or higher. Details of the child patient and family respondent characteristics can be found in Table 1.
Table 1
| Variable | Values |
|---|---|
| Child patient | |
| Age (years) | |
| 3–6 | 357 (35.3) |
| 7–9 | 278 (27.5) |
| 10–12 | 224 (22.2) |
| 13–17 | 151 (15.0) |
| Gender | |
| Male | 598 (59.2) |
| Female | 412 (40.8) |
| Global health status | |
| Poor or fair | 64 (6.3) |
| Good | 72 (7.1) |
| Very good | 373 (36.9) |
| Excellent | 501 (49.6) |
| Family respondent | |
| Age (years) | |
| <25 | 14 (1.4) |
| 25–34 | 327 (32.4) |
| 35–44 | 527 (52.2) |
| ≥45 | 142 (14.1) |
| Education level | |
| Primary school or less | 47 (4.7) |
| Junior high school | 229 (22.7) |
| High school graduate | 192 (19.0) |
| Some college or 2-year degree | 197 (19.5) |
| 4-year college graduate | 292 (28.9) |
| More than 4-year college degree | 53 (5.2) |
| Relationship to the child | |
| Father | 250 (24.8) |
| Mother | 692 (68.5) |
| Grandparents | 28 (2.7) |
| Other | 40 (4.0) |
| National Regional Center for Pediatric | |
| Northeast Center | 170 (16.8) |
| North Center | 211 (20.9) |
| East Center | 140 (13.9) |
| Central South Center | 170 (16.8) |
| Southwest Center | 148 (14.7) |
| Northwest Center | 171 (16.9) |
Data are presented as n (%).
Top-box scores of family caregivers’ experience measures
Table 2 presents Top-box scores for doctor-child communication and global ratings across six NRCP hospitals. The composite score for nurse-child communication ranged from 66.5% to 91.9% at the hospital level. Item-level analysis revealed substantial variation, with listen carefully to child achieved the highest performance (94.6% at the southwest center) compared to the lowest-performing item encourage child to ask questions received the lowest (64.1%, northwest center). The two global rating measures maintained consistently high Top-box scores around 90% in total, higher than the 85.5% composite score observed for doctor-child communication.
Table 2
| NRCP | How well doctors communicate with your child | Global ratings | |||||
|---|---|---|---|---|---|---|---|
| Listen carefully to child | Easy for child to understand | Encourage child to ask questions | Composite measure | Overall rating of hospital | Willingness to recommend the hospital | ||
| Northeast Center | 85.3 | 85.9 | 85.3 | 85.5 | 90.0 | 83.5 | |
| North Center | 88.6 | 86.3 | 85.3 | 86.7 | 93.8 | 94.8 | |
| East Center | 82.1 | 80.7 | 80.0 | 81.0 | 89.3 | 97.1 | |
| Central South Center | 77.2 | 76.6 | 72.5 | 75.4 | 85.4 | 87.1 | |
| Southwest Center | 94.6 | 92.6 | 90.5 | 92.6 | 96.6 | 98.0 | |
| Northwest Center | 70.6 | 72.9 | 64.1 | 69.2 | 75.3 | 82.9 | |
| Total | 83.1 | 82.5 | 79.6 | 85.5 | 88.4 | 90.4 | |
Data are presented as %. NRCP, National Regional Center for Pediatric.
Associations between doctor-child communication and caregivers’ evaluations of hospital care
The internal consistency of the three communication items was excellent (Cronbach’s α=0.924), with item-total correlations ranging from 0.927 to 0.948. Removal of any item reduced the overall α coefficient.
Table 3 presents the associations between doctor-child communication and caregivers’ overall hospital ratings. In both the unadjusted and adjusted models, encouraging the child to ask questions was significantly associated with higher overall ratings (unadjusted β=1.149, 95% CI: 0.241–2.056, P<0.05; adjusted β=1.075, 95% CI: 0.141–2.009, P<0.05). Listening carefully to the child was significantly associated with overall ratings in the unadjusted model (β=1.367, 95% CI: 0.016–2.718, P<0.05) but not in the adjusted model. Explaining in a way the child could understand was not significantly associated with overall ratings in either model.
Table 3
| Doctor-child communication | β (95% CI) | |
|---|---|---|
| Overall rating of hospital (independent variables only) | Overall rating of hospital including covariates | |
| Independent variables | ||
| Listen carefully to child | 1.367 (0.016, 2.718)* | 1.201 (−0.189, 2.592) |
| Easy for child to understand | 0.589 (−0.861, 2.039) | 0.412 (−1.090, 1.915) |
| Encourage child to ask questions | 1.149 (0.241, 2.056)* | 1.075 (0.141, 2.009)* |
| Covariates | ||
| Child global health status | ||
| Poor or fair | Reference | |
| Good | 1.102 (−1.004, 3.209) | |
| Very good | 1.910 (−0.249, 4.070) | |
| Excellent | 2.424 (0.383, 4.464)* | |
| Respondent relationship to the child | ||
| Father | Reference | |
| Mother | 0.430 (−0.143, 1.003) | |
| Grandparents | −0.056 (−1.368, 1.255) | |
| Other | −0.049 (−1.081, 0.984) | |
| Effect size | ||
| AIC | 737.70 | 727.99 |
| McFadden R2 | 0.161 | 0.186 |
α levels of significance: *P<0.05. AIC, Akaike information criterion; CI, confidence interval.
Among covariates, child global health status of “Excellent” was significantly associated with higher overall hospital ratings in the adjusted model (β=2.424, 95% CI: 0.383–4.464, P<0.05), while other health status categories and respondent relationship to the child were not significantly associated. Model fit improved after inclusion of covariates [Akaike information criterion (AIC) decreased from 737.70 to 727.99; McFadden’s R2 increased from 0.161 to 0.186].
Table 4 shows the associations between doctor-child communication and caregivers’ willingness to recommend the hospital. Consistent with the findings for overall ratings, encouraging the child to ask questions was the only communication variable significantly associated with recommendation intention, and the association was positive (unadjusted β=1.485, 95% CI: 0.571–2.400, P<0.01; adjusted β=1.382, 95% CI: 0.425–2.339, P<0.01). The other communication variables (listening carefully to the child and explaining in a way the child could understand) were not statistically significant in either the unadjusted or adjusted model.
Table 4
| Doctor-child communication | β (95% CI) | |
|---|---|---|
| Willingness to recommend the hospital (independent variables only) | Willingness to recommend the hospital including covariates | |
| Independent variables | ||
| Listen carefully to child | 1.041 (−0.303, 2.385) | 1.030 (−0.395, 2.455) |
| Easy for child to understand | −0.203 (−1.811, 1.405) | −0.645 (−2.331, 1.041) |
| Encourage child to ask questions | 1.485 (0.571, 2.400)** | 1.382 (0.425, 2.339)** |
| Covariates | ||
| Child global health status | ||
| Poor or fair | Reference | |
| Good | 0.061 (−2.324, 2.446) | |
| Very good | 0.957 (−1.480, 3.394) | |
| Excellent | 1.832 (−0.516, 4.181) | |
| Respondent relationship to the child | ||
| Father | Reference | |
| Mother | 0.237 (−0.361, 0.835) | |
| Grandparents | −0.206 (−1.515, 1.104) | |
| Other | −0.087 (−1.130, 0.957) | |
| Effect size | ||
| AIC | 691.62 | 672.18 |
| McFadden R2 | 0.118 | 0.159 |
α levels of significance: **P<0.01. AIC, Akaike information criterion; CI, confidence interval.
Child global health status and respondent relationship to the child were not significantly associated with recommendation willingness in the adjusted model. Model fit improved after covariate adjustment (AIC decreased from 691.62 to 672.18; McFadden’s R2 increased from 0.118 to 0.159).
Ordinal communication variables were decomposed into orthogonal polynomial contrasts, and only the linear term was reported as the primary effect because quadratic and cubic terms were not robust across adjusted models.
Cross-sectional path analysis of associations
An exploratory path analysis was conducted to examine the pattern of statistical associations between doctors encouraging children to ask questions and family caregivers’ willingness to recommend the hospital, with overall hospital rating as an intervening variable (Figure 2). The indirect association through overall hospital rating was β=0.338 (95% CI: 0.206–0.471, P<0.001), accounting for approximately 57.81% of the total statistical association. The path model demonstrated an overall acceptable fit to the data (χ2=40.895, df =5, P<0.001). The CFI was 0.991 and the TLI was 0.933, indicating good model fit. The RMSEA was 0.084, and the SRMR was 0.037, both within acceptable ranges.

Discussion
Key findings
The present study aimed to explore doctor-child communication and its impact on caregivers’ recommendation willingness and overall hospital ratings. Our retrospective, multicenter analysis of 1,010 caregivers’ experience data from six National Regional Centers for Pediatric in China provides empirical data to bridge these gaps. Encouraging the child to ask questions was significantly associated with higher overall hospital ratings, consistent with prior research indicating that effective communication is positively related to patient satisfaction (29,30). Notably, this was also the only communication component that demonstrated a significant independent association with caregivers’ willingness to recommend the hospital, a relationship that has been less consistently reported in previous studies. Furthermore, the child’s perceived global health status was identified as a powerful covariate, influencing both outcome measures, consistent with the notion that the patient’s health condition is a fundamental factor in healthcare evaluation (31). We found that overall hospital rating partially mediated the association between encouraging the child to ask questions and caregivers’ willingness to recommend the hospital, accounting for 57.81% of the total effect. These findings contribute to a more nuanced understanding of caregivers’ experiences in pediatric care settings.
Strengths and limitations
This study has several strengths, including a large multicenter sample from China’s top-tier pediatric hospitals, the use of the validated Child HCAHPS instrument for international benchmarking, and an in-depth analysis that dissects specific communication behaviors and their exploratory path-analytic associations. However, its cross-sectional design precludes definitive causal inferences, calling for future longitudinal or experimental research to establish causality and understand the temporal dynamics of communication. While key covariates were adjusted for, residual confounding from unmeasured factors like clinical severity and clinician workload may persist, necessitating the incorporation of objective measures in subsequent studies. The reliance on caregiver-reported data introduces potential subjective bias, underscoring the need for qualitative or mixed-methods approaches to deeply explore underlying mechanisms from both caregiver and child perspectives. Finally, as the findings are rooted in China’s specific healthcare context, future work should test the proposed interventions and the model’s generalizability across diverse cultural and healthcare systems.
Comparison with similar research
Our findings both align with and extend existing literature. While the positive link between overall communication quality and hospital ratings reaffirms communication’s central role in pediatric care (5), we found distinct communication behaviors differentially impact evaluation dimensions. This complexity reflects the recognized distinction between affective and instrumental communication behaviors (32), and parallels findings that specific communication failures strongly undermine both perceived care quality and patient loyalty (33).
Furthermore, our observed mediation association reveals a dual-pathway psychological mechanism. Positive communication experiences enhance the overall perception of the hospital, which subsequently strengthens the intention to recommend it (34).
Explanations of findings
The predictive power of encourage child to ask questions on caregivers’ willingness to recommend the hospital, underline the behavior goes beyond simple information exchange; it represents a deeper level of empowerment and respect for the child’s agency within the triadic medical encounter (35). In pediatric settings, caregivers are highly sensitive to how healthcare providers interact with their children. An action that promotes child participation, such as encouraging questions, can be seen as a proxy for patient-centered care, which in turn fosters trust and emotional security for the entire family (36). This finding resonates with a broader consensus in service research: that in high-stakes contexts like healthcare, where outcomes can be uncertain, the quality of interpersonal communication is not merely supportive but a critical determinant of the service experience (37). It underscores that fine-tuned, patient-centered communication serves as a fundamental mechanism to navigate uncertainty, build trust, and ultimately define the perceived quality of care.
Physician communication that is empathetic and child-centered transforms care experiences and directly impacts caregiver evaluations. Furthermore, while clinical outcomes are a foundational determinant of satisfaction (38), effective communication is indispensable for maintaining trust amid uncertainty (39,40) and overcoming barriers to treatment adherence (41), thereby uniting clinical excellence and communication as the cornerstone of pediatric care.
Implication
This study provides actionable strategies for enhancing pediatric communication. Training must prioritize techniques to actively encourage children’s questions, moving beyond basic listening and explanation skills. This approach acknowledges the triadic nature of pediatric care, where empowering the child simultaneously addresses caregiver needs (42). Furthermore, systemic support is crucial. Institutions should integrate dedicated roles (e.g., Child Life Specialists) to manage routine support, develop family-friendly educational materials, and protect adequate consultation time to enable meaningful, unhurried interactions (43).
Conclusions
This multicenter study establishes that effective doctor-child communication, particularly the distinct role of encouraging children’s questions, significantly enhances both hospital ratings and recommendation willingness. The findings reveal a key psychological pathway where overall perceptions mediate this relationship, even after accounting for the child’s health status. To translate this into practice, healthcare institutions should prioritize fostering a communication environment that actively promotes child engagement, supported by targeted clinician training and necessary systemic adjustments.
Acknowledgments
None.
Footnote
Reporting Checklist: The authors have completed the STROBE reporting checklist. Available at https://tp.amegroups.com/article/view/10.21037/tp-2025-1-887/rc
Data Sharing Statement: Available at https://tp.amegroups.com/article/view/10.21037/tp-2025-1-887/dss
Peer Review File: Available at https://tp.amegroups.com/article/view/10.21037/tp-2025-1-887/prf
Funding: None.
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://tp.amegroups.com/article/view/10.21037/tp-2025-1-887/coif). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The study was conducted in accordance with the Declaration of Helsinki and its subsequent amendments. The ethical approval was obtained from the Ethics Committee of the Institute of Medical Information, Chinese Academy of Medical Sciences and Peking Union Medical College (No. IMICAMS/04/19/HREC) and individual consent for this retrospective analysis was waived.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Yagiela LM, Carlton EF, Meert KL, et al. Parent Medical Traumatic Stress and Associated Family Outcomes After Pediatric Critical Illness: A Systematic Review. Pediatr Crit Care Med 2019;20:759-68. [Crossref] [PubMed]
- Bhandari MM, Abbasi A, Bhatt V. The effect of hospitalization on children: a review of psychological, social, and developmental impacts. Indian Journal of Surgical Nursing 2025;14:19-22.
- Paron K, Kutsar D. Creation of child-patient’s autonomy in a child-parent-doctor relationship: Medical doctors’ perspectives. Childhood 2023;30:145-60.
- Yuan S, Humphris G, MacPherson LMD, et al. Communicating With Parents and Preschool Children: A Qualitative Exploration of Dental Professional-Parent-Child Interactions During Paediatric Dental Consultations to Prevent Early Childhood Caries. Front Public Health 2021;9:669395. [Crossref] [PubMed]
- Lee T, Cui J, Rosario H, et al. Assessment of caregiver expectations of physician communication in a pediatric setting. BMC Health Serv Res 2020;20:408. [Crossref] [PubMed]
- Alanezi S. A modified framework for understanding provider–patient communication in healthcare. International Journal of Advanced and Applied Sciences 2025;12:100-7.
- Beckett MK, Quigley DD, Cohea CW, et al. Trends in HCAHPS Survey Scores, 2008-2019: A Quality Improvement Perspective. Med Care 2024;62:416-22. [Crossref] [PubMed]
- Hui EK, Tsang SK. Self-determination as a psychological and positive youth development construct. ScientificWorldJournal 2012;2012:759358. [Crossref] [PubMed]
- Henry N, Montgomery E, Ghosh P, et al. Caregiver inclusion influence on adolescent acceptance and engagement of an mHealth app, a randomized controlled trial. Mhealth 2025;11:57. [Crossref] [PubMed]
- Chen SX, Wu HC, Cheng D. The Influences of Immersive Sensory Cues on Immersive Experience Recommendation Intentions in a Digital Exhibition: A Cognitive-Affective-Conative Model. Event Management 2025;29:131-48.
- Sultan S, Duval M, Aramideh J, et al. Training healthcare professionals in hypnosis-derived communication to mitigate procedural pain in children. Sci Rep 2025;15:8266. [Crossref] [PubMed]
- Glick AF, Farkas JS, Magro J, et al. Management of Discharge Instructions for Children With Medical Complexity: A Systematic Review. Pediatrics 2023;152:e2023061572. [Crossref] [PubMed]
- Sisk BA, Friedrich AB, Kaye EC, et al. Multilevel barriers to communication in pediatric oncology: Clinicians' perspectives. Cancer 2021;127:2130-8. [Crossref] [PubMed]
- Ye J, Yang L, Axelin A, et al. The implementation and strategy of triadic communication in pediatric oncology: a scoping review. Pediatr Res 2025;97:1803-22. [Crossref] [PubMed]
- Sisk BA, Friedrich A, Blazin LJ, et al. Communication in Pediatric Oncology: A Qualitative Study. Pediatrics 2020;146:e20201193. [Crossref] [PubMed]
- Hodgson CR, Mehra R, Franck LS. Child and Family Outcomes and Experiences Related to Family-Centered Care Interventions for Hospitalized Pediatric Patients: A Systematic Review. Children (Basel) 2024;11:949. [Crossref] [PubMed]
- Woldring JM, Luttik ML, Paans W, et al. The added value of family-centered rounds in the hospital setting: A systematic review of systematic reviews. PLoS One 2023;18:e0280142. [Crossref] [PubMed]
- Spataro V, Corazza I, Hazelzet JA, et al. A systematic literature review on initiatives to involve children and adolescents in evaluating their hospitalization experience. BMC Health Serv Res 2025;25:429. [Crossref] [PubMed]
- Ahmed S, Kemp K, Johnson D, et al. Identifying areas for improvement in paediatric inpatient care using the Child HCAHPS survey. Paediatr Child Health 2020;25:365-71. [Crossref] [PubMed]
- Campbell K, Cunningham S, Neeley A, et al. Ratings of Physician Communication by Caregivers of Hospitalized Children With and Without Autism. Hosp Pediatr 2021;11:547-53. [Crossref] [PubMed]
- Parente VM, Nagy G, Pollak KI. Patient- and Family-Centered Hospital Care-The Need for Structural Humility. JAMA Pediatr 2023;177:553-4. [Crossref] [PubMed]
- Pei C, Han X, Liu Q, et al. Case-mix adjustment of patient-reported experience measures in National Regional Center for Pediatric. Pediatr Res 2023;94:1562-9. [Crossref] [PubMed]
- Martino SC, Reynolds KA, Grob R, et al. Evaluation of a protocol for eliciting narrative accounts of pediatric inpatient experiences of care. Health Serv Res 2023;58:271-81. [Crossref] [PubMed]
- Hu G, Yuan C, Ren H, et al. Reliability and validity of an instrument to assess pediatric inpatients' experience of care in China. Transl Pediatr 2021;10:2269-80. [Crossref] [PubMed]
- Weng Y, Pei C, Liu Q, et al. Association between nurse-child communication and family caregivers' global ratings to hospital: a retrospective study. J Pediatr Nurs 2024;78:e424-31. [Crossref] [PubMed]
- Labrague LJ, de Los Santos JAA. Resilience as a mediator between compassion fatigue, nurses' work outcomes, and quality of care during the COVID-19 pandemic. Appl Nurs Res 2021;61:151476. [Crossref] [PubMed]
- Peng Y, Wang Y, Huang W, et al. Exploring Perceptions and Barriers: A Health Belief Model-Based Analysis of Seasonal Influenza Vaccination among High-Risk Healthcare Workers in China. Vaccines (Basel) 2024;12:796. [Crossref] [PubMed]
- Schwartz Tayri TM, Dahan Heller E, Gal A. The Role of Supervision in Enhancing Social Workers' Professional Resilience. Soc Work 2026;swag002. [Crossref] [PubMed]
- Chen S, Guo X, Wu T, Ju X. Exploring the Online Doctor-Patient Interaction on Patient Satisfaction Based on Text Mining and Empirical Analysis. Information Processing & Management 2020;57:102253.
- Li L, Cui X, Feng W. Enhancing Patient Satisfaction in Cross-Regional Healthcare: a Cross-Sectional Study in the Knowledge-Based Healthcare Landscape. Journal of the Knowledge Economy 2024;15:14172-98.
- Bakhtiarvand SZ, Rahaei Z, Sadeghian HA, et al. The constructs of health literacy in children: a systematic review. BMC Public Health 2025;25:3352. [Crossref] [PubMed]
- Bockes A, Hebart MN, Lingnau A. Revealing Key Dimensions Underlying the Recognition of Dynamic Human Actions. Commun Psychol 2025;3:149. [Crossref] [PubMed]
- Clark R, Klaiman T, Sliwinski K, et al. Communication failures and racial disparities in inpatient maternity care: a qualitative content analysis of incident reports. BMJ Open Qual 2025;14:e003112. [Crossref] [PubMed]
- Chen X, Liu C, Yan P, et al. The impact of doctor-patient communication on patient satisfaction in outpatient settings: implications for medical training and practice. BMC Med Educ 2025;25:830. [Crossref] [PubMed]
- van Woerden CS, Vroman H, Brand PLP. Child participation in triadic medical consultations: A scoping review and summary of promotive interventions. Patient Educ Couns 2023;113:107749. [Crossref] [PubMed]
- Haine-Schlagel R, Dickson KS, Lind T, et al. Caregiver Participation Engagement in Child Mental Health Prevention Programs: a Systematic Review. Prev Sci 2022;23:321-39. [Crossref] [PubMed]
- Danaher TS, Berry LL, Howard C, et al. Improving How Clinicians Communicate With Patients: An Integrative Review and Framework. Journal of Service Research 2023;26:493-510.
- Ferreira DC, Vieira I, Pedro MI, et al. Patient Satisfaction with Healthcare Services and the Techniques Used for its Assessment: A Systematic Literature Review and a Bibliometric Analysis. Healthcare (Basel) 2023;11:639. [Crossref] [PubMed]
- Kerr AM, Harrington NG, Scott AM. Communication and the Appraisal of Uncertainty: Exploring Parents' Communication with Credible Authorities in the Context of Chronic Childhood Illness. Health Commun 2019;34:201-11. [Crossref] [PubMed]
- Kerr AM, Thompson CM, Stewart CA, et al. "I Want Them to Still Trust Me with Their Child's Care": A Longitudinal Study of Pediatric Residents' Reactions to and Communication with Parents about Medical Uncertainty across Residency. Health Commun 2023;38:1054-64. [Crossref] [PubMed]
- Simon M, Danner S, Saavedra S, et al. The Complex Interplay of Communication and Trust in Healthcare Delivery. Harv Public Health Rev (Camb) 2021;39: [Crossref] [PubMed]
- Lenne E, Sun CJ, Klawetter S. An Examination of Power in a Triadic Model of Parent-Child-Pediatrician Relationships Related to Early Childhood Gender Development. J Fam Theory Rev 2023;15:662-76. [Crossref] [PubMed]
- Rosenblatt A, Pederson R, Davis-Sandfoss T, et al. Child life specialist services, practice, and utilization across health care: a scoping review. JBI Evid Synth 2024;22:1303-28. [Crossref] [PubMed]