A retrospective cohort study on clinical features of foreign bodies in the gastrointestinal tract of children—emergency data from a pediatric regional medical center in eastern China
Highlight box
Key findings
• This study represents the largest single-center report in China over the past three years. Key findings include: a complication rate of 20.9%, higher than contemporaneous reports from Europe and the United States (10–15%), suggesting a higher proportion of delayed medical presentation in China; coins remained the most common foreign body (63.2%), but the proportions of button batteries (15.7%) and magnetic beads (10.7%) were significantly higher than in pre-2015 domestic data (both <5%), reflecting new trends toward electronic and miniaturized toys.
What is known and what is new?
• Gastrointestinal foreign body tracts of children can trigger a cascade of severe complications, including ulcers, perforations, bleeding, mediastinal infections, and even rupture of major blood vessels. These events not only prolong hospital stays and double medical costs but also impose a heavy psychological and economic burden on families and society alike.
• We are the first to propose a dual-threshold warning based on ‘retention site + retention time’: the risk of complications is 3.61 times higher when the retention site is in the upper segment of the esophagus compared to retention at other sites, and 4.56 times higher when the retention time exceeds 24 hours compared to a retention time of 24 hours or less, which can serve as a ‘red flag’ for regional referral. This provides feasibility evidence for subsequent prospective randomized controlled trials.
What is the implication, and what should change now?
• The research findings imply: primary hospitals can use the ‘age <4 years + upper esophagus + retention time >24 hours’ three-factor standard, avoiding secondary transfers; regional medical centers should establish an ‘high-risk foreign body list’ and push it instantly to kindergartens and family doctors, achieving primary prevention; endoscopy centers need to set up ‘battery/magnetic bead emergency slots’ to ensure removal within 6 hours, reducing the perforation rate from 18.4% to less than 5%.
Introduction
Foreign bodies in the gastrointestinal tract are one of the common emergencies in pediatric emergency care, referring to various objects that cannot be digested and remain in the gastrointestinal tract without being promptly expelled. They are also one of the critical and urgent conditions frequently encountered in gastroenterology (1). Children account for 70–80% of all cases of gastrointestinal foreign body (GIFB) ingestion worldwide, these foreign bodies can lead to severe complications such as gastrointestinal mucosal ulcers, obstruction or perforation, peritonitis, sepsis, and even rupture of major blood vessels, resulting in the child’s death (2). The annual incidence of GIFB in children worldwide is approximately 12–16 cases per 100,000 children. According to a 2022 report by the American College of Emergency Physicians, there were 102,000 cases of GIFB in children under 14 years old, with a complication rate of 8.9%; the multi-center data from the European Society for Paediatric Gastroenterology, Hepatology, and Nutrition (ESPGHAN) showed a complication rate of 11.4% (3). In China, single-center reports of pediatric GIFB complication rates range from 9% to 26%, with substantial variability attributed to regional clinical practice differences.
This paper presents a retrospective analysis of cases of GIFB treated in the emergency department of a children’s regional medical center in eastern China. It summarizes the characteristics of these cases and their complications, conducts a statistical analysis of the relevant risk factors, and aims to provide reference for clinical diagnosis and treatment. We present this article in accordance with the STROBE reporting checklist (available at https://tp.amegroups.com/article/view/10.21037/tp-2026-1-0009/rc).
Methods
Study design
This study included case data from the Emergency Department of the Children’s Hospital of Zhejiang University School of Medicine from October 2021 to October 2024, with all data sourced from the hospital’s electronic medical record (EMR) system. Researchers retrospectively extracted data by grouping based on different characteristics such as the child’s age, gender, foreign body risk level (2,4), number of foreign bodies, location of foreign body retention, duration of foreign body retention, method of ingestion, presence of comorbidities, and whether complications occurred. The study was conducted in accordance with the Declaration of Helsinki and its subsequent amendments. The study was approved by Medical Ethics Committee of the Children’s Hospital, Zhejiang University School of Medicine (No. 2025-IRB-0115-P-01) and individual consent for this analysis was waived due to the retrospective nature.
Setting
The study was conducted in the Emergency Department of Children’s Hospital, Zhejiang University School of Medicine, a tertiary pediatric referral center serving Hangzhou and surrounding regions in eastern China. The study period spanned from October 1, 2021, to October 31, 2024 (37 months). During this period, the Emergency Department maintained standardized protocols for suspected foreign body ingestion including immediate radiographic evaluation and pediatric gastroenterology consultation. Data for all eligible cases were retrospectively extracted from EMRs, with all patients followed until foreign body resolution and hospital discharge as documented in clinical records.
Participants
Eligibility criteria
We included all children aged 0–18 years presenting to the emergency department with confirmed GIFB ingestion supported by clinical history and objective evidence [X-ray, computed tomography (CT), or endoscopic confirmation]. All cases were admitted through the emergency department with documented ingestion history.
Exclusion criteria
We excluded: (I) children with incomplete clinical data precluding analysis; (II) respiratory tract foreign bodies; (III) unconfirmed ingestion cases; and (IV) patients leaving against medical advice (LAMA) before treatment completion.
Participant selection
We identified potential cases from the EMR system using ICD-10 codes T18.0-T18.9 and emergency admission logs. Two researchers (Y.H., J.L.) independently screened records for eligibility. Of 798 initially identified cases, 72 were excluded: 40 due to incomplete data, 18 respiratory foreign bodies, 9 unconfirmed cases, and 5 patients with LAMA, leaving 726 participants for analysis.
Variables
Outcomes
The primary outcome was complication occurrence, defined as any of: gastrointestinal ulceration, perforation, esophagitis, gastritis, bleeding, obstruction, or mediastinitis during hospital stay, diagnosed by clinical findings, endoscopy, or radiography. Secondary outcomes included surgical intervention requirement and hospital length of stay.
Exposures
- Age: categorized as <4 vs. ≥4 years based on clinical significance and previous literature (5-7).
- Foreign body type: classified by risk level—low (coins, smooth plastic, rubber), medium (single magnetic bead, smooth plastic blocks), or high (button batteries, multiple magnets ≥2, sharp metal) per national guidelines (8,9).
- Number: single vs. multiple (≥2) foreign bodies.
- Retention location: upper esophagus vs. other gastrointestinal sites.
- Retention time: time from reported ingestion to removal/expulsion, dichotomized at 24 hours (≤24 h =0, >24 h =1) based on clinical guidelines (8,9).
- Ingestion method: accidental vs. intentional (deliberate ingestion reported by child/caregiver).
- Mental disorder comorbidity: documented psychiatric diagnoses [e.g., trichophagia, developmental disorders, autism spectrum disorder (ASD), intellectual disability (ID)].
Potential confounders
Age, gender, foreign body type, number, retention location, retention time, ingestion method, and mental disorder comorbidity were considered based on literature review.
Effect modifiers
We examined potential effect modification by age group on the association between high-risk foreign bodies and complications.
Data sources and measurement
Data were extracted from the hospital’s Epic EMR system, which includes clinical documentation, imaging reports, endoscopy records, and discharge summaries. Two researchers independently extracted data using standardized forms, with discrepancies resolved by senior author (Y.Z.) discussion. For quality assurance, 10% of records were randomly selected for cross-checking against original medical records, showing >95% agreement.
- Demographics: age, gender, admission date from admission records.
- Clinical presentation: symptoms and ingestion time from emergency notes.
- Imaging: foreign body location, number, type from radiology reports.
- Endoscopy: removal method, mucosal findings from endoscopy reports.
- Outcomes: complications, interventions from progress notes and discharge summaries.
- Mental health: documented psychiatric diagnoses from medical history.
Bias
We identified and addressed several potential biases:
- Selection bias: we minimized selection bias by including all consecutive eligible cases. However, as a tertiary referral center, we may have preferentially included more severe cases, potentially overestimating complication rates compared to primary care settings. This is discussed as a limitation;
- Information bias: to reduce misclassification, we used objective imaging and endoscopic findings rather than relying solely on history. For retention time, we used the earliest reported ingestion time, acknowledging potential caregiver recall bias. Ten percent of imaging studies were independently reviewed by a pediatric radiologist blinded to outcomes to assess diagnostic accuracy;
- Detection bias: all patients received standardized imaging protocols, minimizing differential detection. However, patients with more severe symptoms may have received more intensive monitoring, potentially increasing complication detection in high-risk groups. It should be noted that this study has a significant detection bias: the high endoscopy rate (72.3%) led to a higher diagnosis rate of complications such as esophagitis and gastritis (only diagnosable via endoscopy), while the conservative group could not be diagnosed with these complications, resulting in an overestimation of the overall complication rate (20.9%). In addition, as a tertiary pediatric referral center, our study included more severe cases, which is another reason why the complication rate is higher than that of Western studies (10–15%);
- Confounding: we addressed potential confounding through multivariate logistic regression adjustment for all a priori identified confounders.
Study size
The study size was determined by the available cases during the 37-month study period. Based on previous annual volumes of approximately 250 foreign body ingestions per year, we anticipated 750–800 cases. A post-hoc power calculation with 726 participants (152 with complications, 574 without) indicated >80% power to detect an odds ratio (OR) of 1.5 for common exposures (prevalence >20%) at α=0.05.
Quantitative variables
Age was categorized as <4 vs. ≥4 years based on established clinical relevance. Retention time was dichotomized at 24 hours per clinical guidelines. In sensitivity analyses, we also examined retention time as continuous (log-transformed) and using alternative cutoffs (12, 24, 48 hours).
Statistical methods
Primary analysis
Using SPSS 26.0, we compared categorical variables by χ2 test or Fisher’s exact test and continuous variables by t-tests. Multivariate logistic regression identified independent risk factors for complications, adding an interaction term between age group (<4/≥4 years) and ingestion method (accidental/intentional) to the multivariate logistic regression model to account for clinically inseparable factors, and tested the significance of the interaction term with likelihood ratio test, adjusting for all potential confounders. We reported OR with 95% confidence intervals (CI). Two-tailed P<0.05 was considered significant.
Missing data
Missing data were minimal (<5% for all variables). We performed complete case analysis and conducted sensitivity analyses using multiple imputation by chained equations (MICE) with 10 datasets to assess robustness.
Subgroup analyses
We performed stratified analyses by age group (<4 vs. ≥4 years) and tested for interactions between age and each risk factor.
Sensitivity analyses
We conducted four sensitivity analyses: (I) excluding children with mental disorders; (II) using different retention time cutoffs (12, 24, 48 hours); (III) restricting to high-risk foreign bodies only; and (IV) using propensity score matching to balance covariates.
Results
Participants
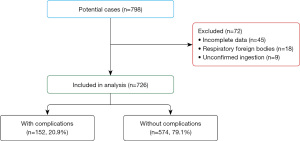
During the study period, we identified 798 children with suspected GIFB. After applying inclusion and exclusion criteria, 726 children were included (Figure 1). Exclusions were: 45 incomplete data, 18 respiratory foreign bodies, and 9 unconfirmed cases. All 726 included participants were followed until foreign body resolution and discharge.
General clinical data of patients and univariate analysis
This study included a total of 726 pediatric patients with GIFB admitted to the Emergency Department of the Children’s Hospital Affiliated to Zhejiang University School of Medicine from October 2021 to October 2024. In terms of gender distribution, there were 428 male cases (59.00%) and 298 female cases (41.00%). Regarding age distribution: 397 cases (54.70%) were children under 4 years old, and 329 cases (45.30%) were children aged 4 years or older. Among 726 cases, most patients recovered well after treatment, while 152 cases (20.9%) developed complications. Specifically, 68 cases (44.7% of the complications) presented with gastrointestinal ulcers, commonly occurring at sites where foreign bodies were retained; 28 cases (18.4%) experienced perforation, and 56 cases (36.9%) had esophagitis/gastritis. No deaths were observed in this cohort. The clinical characteristics of complicated pediatric GIFB cases are shown in Table 1.
Table 1
| Foreign body type | Impaction location | Time to removal (hours) | Retention time (hours) | Hospital stay (days) | Acute complication | Late complication |
|---|---|---|---|---|---|---|
| Button battery | Upper esophagus | 1.2±0.5 | 3.5±1.2 | 7.8±2.3 | Perforation/ulcer | Esophageal stenosis |
| Multiple magnets | Stomach/duodenum | 4.5±1.8 | 6.8±2.5 | 6.5±2.1 | Ulcer/obstruction | None |
| Sharp metal | Esophagus/ileum | 2.8±1.1 | 4.2±1.5 | 8.2±2.5 | Perforation/bleeding | Ileal stricture |
| Coins | Upper esophagus | 12.5±3.6 | 24.8±5.2 | 3.1±1.0 | Esophagitis/gastritis | None |
| Others | Various | 18.6±4.2 | 30.5±6.8 | 4.5±1.5 | Gastritis/obstruction | None |
Data are presented as mean ± SD. GIFB, gastrointestinal foreign body; SD, standard deviation.
Types of foreign bodies (classified by risk level)
Low-risk foreign bodies numbered 450 cases (62.00%), the highest proportion, with common types including coins, smooth plastic beads, and rubber products without sharp edges; medium-risk foreign bodies totaled 152 cases (21.00%), such as single magnetic beads and smooth plastic blocks; high-risk foreign bodies were 124 cases (17.00%), mainly including button batteries 114 cases, multiple magnetic beads 7 cases, and sharp metal foreign bodies (such as sewing needles) one case.
Stagnation sites
Among 296 cases (40.80%), foreign bodies were retained in the upper esophagus; the remaining 430 cases (59.20%) were retained in other digestive tract regions outside the esophagus (including the stomach, small intestine, large intestine, etc.). The primary retention site was non-esophageal regions, with the upper esophagus being the most common site of retention within the esophagus. Among all the children, 664 cases (91.50%) had the foreign body removed or naturally expelled from the body within 24 hours of its entry; 62 cases (8.50%) had a retention time exceeding 24 hours, with an average retention time of (14.2±9.6) hours.
Route of intake
Accidental ingestion accounted for 667 cases (91.90%); intentional swallowing accounted for 59 cases (8.13%), mainly among older children, with some related to abnormal mental and behavioral conditions. Among these, 80 cases (11.02%) had comorbid mental disorders. The probability of GIFB complications in children with comorbid mental disorders was 37.50% (30/80), significantly higher than that in children without comorbid mental disorders at 18.89% (122/646).
Treatment methods
Endoscopic removal of foreign bodies via esophagogastroduodenoscopy (EGD) was performed in 525 cases (72.30%), serving as the primary intervention; 192 cases (26.40%) expelled foreign bodies naturally through the intestines after conservative treatment, mostly involving low-risk, small-sized foreign bodies; only 9 cases (1.30%) required surgical intervention due to severe foreign body impaction or combined perforation.
The results of univariate analysis showed that there was no statistically significant difference between the group without complications and the group with complications in terms of gender, type of foreign body, number of foreign bodies, and removal method (all P values >0.05). However, age (P=0.009), location of foreign body retention (P<0.001), retention time (P<0.001), ingestion method (P=0.006), and whether combined with mental disorders (P=0.006) were influencing factors for the occurrence of complications in children with digestive tract foreign bodies, as shown in Table 2.
Table 2
| Characteristics | Group with complications (n=152) | Group without complications (n=574) | χ2 value | P value |
|---|---|---|---|---|
| Gender | 0.001 | 0.97 | ||
| Male | 89 (58.5) | 339 (59.1) | ||
| Female | 63 (41.5) | 235 (40.9) | ||
| Age (years) | 6.91 | 0.009 | ||
| <4 | 95 (62.5) | 302 (52.6) | ||
| ≥4 | 57 (37.5) | 272 (47.4) | ||
| Risk level (type of foreign body) | 3.077 | 0.08 | ||
| Low | 94 (61.8) | 356 (62.0) | ||
| Medium | 32 (21.1) | 120 (20.9) | ||
| High | 26 (17.1) | 98 (17.1) | ||
| Number of foreign bodies | 1.239 | 0.27 | ||
| 1 | 140 (92.1) | 529 (92.2) | ||
| ≥2 | 12 (7.9) | 45 (7.8) | ||
| Location of foreign body retention | 32.239 | <0.001 | ||
| Upper esophagus | 91 (60.0) | 205 (35.7) | ||
| Others | 61 (40.0) | 369 (64.3) | ||
| Retention time | 22.448 | <0.001 | ||
| ≤24 h | 115 (75.7) | 549 (95.7) | ||
| >24 h | 37 (24.3) | 25 (4.3) | ||
| Entry method | 7.452 | 0.006 | ||
| Accidental ingestion | 128 (84.2) | 539 (93.9) | ||
| Voluntarily swallowing | 24 (15.8) | 35 (6.1) | ||
| Mental disorder | 7.563 | 0.006 | ||
| No | 122 (80.3) | 524 (91.3) | ||
| Yes | 30 (19.7) | 50 (8.7) | ||
| Removal method | 0.325 | 0.57 | ||
| EGD | 110 (72.4) | 415 (72.3) | ||
| Observation | 40 (26.3) | 152 (26.5) | ||
| Operation | 2 (1.3) | 7 (1.2) |
Data are presented as n (%). EGD, esophagogastroduodenoscopy.
Multifactorial logistic regression analysis of complications from foreign bodies in the gastrointestinal tract
Taking the occurrence or non-occurrence of complications as the dependent variable (no =0, yes =1), and age (≥4 years =0, <4 years =1), gender (male =0, female =1), foreign body type (low-risk =0, moderate-risk =1, high-risk =2), number of foreign bodies (single =0, multiple =1), retention location (other sites =0, upper esophagus =1), retention time (≤24 h =0, >24 h =1), ingestion method (accidental ingestion =0, intentional swallowing =1), and whether combined with mental disorders (no =0, yes =1) as independent variables, a multiple logistic regression model was used to analyze and screen for factors related to complications from GIFB. A P value <0.05 indicated statistically significant differences, with a two-tailed test and significance level α=0.05.
The results of multivariate logistic regression analysis for risk factors of complications are presented in Table 3. The results of multivariate analysis showed that age (P=0.009, OR =1.77, 95% CI: 1.156–2.710), retention time of foreign body (>24 h) (P<0.001, OR =4.560, 95% CI: 2.38–8.720), location of foreign body retention (P<0.001, OR =3.613, 95% CI: 2.319–5.629), way of foreign body entry (P=0.006, OR =3.450, 95% CI: 1.290–9.230), and comorbidities of mental disorder (P=0.006, OR =3.780, 95% CI: 1.450–9.860) and the interaction between age <4 years and intentional swallowing (P=0.01, OR =2.438) were risk factors for complications.
Table 3
| Variables | β | SE | P | OR (95% CI) |
|---|---|---|---|---|
| Gender | −0.008 | 0.210 | 0.97 | 0.992 (0.657–1.498) |
| Age | 0.571 | 0.217 | 0.009 | 1.77 (1.156–2.710) |
| Risk level | 0.397 | 0.226 | 0.08 | 1.487 (0.955–2.316) |
| Quantity | 0.496 | 0.446 | 0.27 | 1.642 (0.686–3.933) |
| Location | 1.258 | 0.226 | <0.001 | 3.613 (2.319–5.629) |
| Retention time | 1.519 | 0.321 | <0.001 | 4.56 (2.380–8.720) |
| Entry method | 1.238 | 0.226 | 0.006 | 3.45 (1.290–9.230) |
| Mental disorder | 1.329 | 0.452 | 0.006 | 3.78 (1.450–9.860) |
| Removal method | 0.448 | 0.786 | 0.57 | 1.565 (0.335–7.298) |
| Interaction term between age and ingestion | 0.892 | 0.351 | 0.01 | 2.438 (1.210–4.913) |
CI, confidence interval; GIFB, gastrointestinal foreign body; OR, odds ratio; SE, standard error.
Discussion
Foreign bodies in the gastrointestinal tract can occur at various age stages of childhood, most commonly during the toddler and preschool periods. The results of this study show that the proportion of male patients (59.00%) is significantly higher than that of female patients (41.00%). Children under the age of 4 years account for more than half (54.7%), indicating that infants and young children under 4 years old are a high-risk group for GIFB. This finding is basically consistent with the results reported in domestic and international literature (10-14). The results of the multivariate logistic regression analysis showed that age (P=0.009, OR =1.770, 95% CI: 1.156–2.710) and way of foreign body entry (P=0.006, OR =3.450, 95% CI: 1.290–9.230) were high-risk factors for complications, similar to the results of previous studies (5,15). The cause is often accidental ingestion. Children are very curious, especially younger children who often try to experience new things with their mouths, which leads to the occurrence of accidental swallowing of foreign objects. Moreover, as society and the economy continue to develop, children’s toys keep evolving, introducing items like LEGO sets, super-absorbent gel beads, and electronic products containing button batteries. These innovations have significantly increased the incidence of foreign body ingestion in the digestive tract. Numerous previous surveys have called on parents to keep button batteries and products containing accessible button batteries (such as remote controls) away from young children, or to secure the battery compartments. Some countries impose certain restrictions on the use of magnets in toys; for example, magnetic toys sold in the United Kingdom should bear warnings, and they are even banned in New Zealand (6). Therefore, it is necessary to strengthen education for children and family supervision to prevent foreign body ingestion. It is recommended to establish family education programs to enhance the promotion of knowledge related to foreign bodies, adopting a combination of online and offline methods to improve parents’ and children’s awareness of prevention against foreign bodies.
In this study, the majority of GIFB were retrieved via endoscopy (72.3%), a smaller portion passed naturally through the intestines (26.4%), and only a tiny minority required surgical intervention (1.3%). This result is inconsistent with findings reported in domestic and international literature. In Western countries, most GIFB pass naturally through the intestines, with 10–20% requiring endoscopic treatment, and only 1% of patients needing surgery (5,6,14). Most domestic literature reports that approximately 80% of foreign bodies in children’s gastrointestinal tracts pass through the intestines and are naturally expelled (7-9,16), but there are also reports indicating that endoscopic removal accounts for the highest proportion of GIFB (13,17). The results of the multivariate logistic regression analysis showed that retention time (P<0.001, OR =4.560, 95% CI: 2.38–8.720) and location of foreign body (P<0.001, OR =3.613, 95% CI: 2.319–5.629) are high-risk factors for complications, which are basically consistent with the results reported in domestic and foreign literature (18,19). Due to the presence of anatomical narrow regions within the gastrointestinal tract, such as the three constrictions of the esophagus, the pylorus, the Treitz ligament, the ileocecal valve, and the rectosigmoid junction, coupled with the naturally smaller lumen of children’s digestive tracts, foreign bodies are prone to become lodged. Additionally, some children with congenital gastrointestinal malformations—such as esophageal stenosis, esophageal atresia, swallowing disorders, and achalasia—or those with a history of abdominal surgery are also susceptible to foreign body retention due to the unique conditions of their digestive systems (1). As the retention time of foreign bodies increases, they exert persistent pressure on the local gastrointestinal mucosa, leading to tissue necrosis and thereby increasing the risk of infection. When a foreign body is lodged in the esophagus, especially at the entrance of the esophagus—the first narrow region of the esophagus—where the area is closely connected to surrounding tissues, the foreign body easily compresses the mucosa, causing ischemic necrosis. This compression may even trigger esophageal perforation, a severe complication that requires immediate treatment. In conjunction with clinical practice, as laryngoscopy, gastroscope, and colonoscopy technologies have become more widespread, and to prevent serious complications, most doctors and patients’ families tend to choose endoscopic removal of foreign bodies. Therefore, considering patient safety, timely diagnosis and prompt medical intervention to remove foreign bodies in a timely manner holds great significance for reducing the occurrence of complications, particularly severe ones.
Unlike adults, where foreign bodies primarily include fish bones, chicken bones, and duck bones, children are more likely to ingest objects such as coins, button batteries, magnetic beads and magnets, fruit pits, hair, sewing needles, screws, and date seeds. The risks posed by each type of foreign body are distinctly different (20). The results of this study show that coins are the most common foreign bodies, accounting for 63.2% (459 out of 726) of all cases. However, only 2 cases presented with ulcers, and 5 cases with esophagitis or gastritis, making them the lowest in terms of complications among various types of foreign bodies. In this study, 114 cases involved button batteries (15.7%), with 3 cases of perforation, 34 cases of ulcers, and 21 cases of esophagitis/gastritis (complication rate: 51.7%), which was significantly higher than the overall complication rate (20.9%). Consistent with existing guidelines, emergency endoscopic removal is recommended for button batteries retained in the esophagus, and close monitoring is required for those in the stomach/intestinal tract.
For high-risk foreign bodies (button batteries, multiple magnets ≥2), we strictly followed the ESPGHAN/NASPGHAN guidelines for removal timing: emergency endoscopy (within 2 hours) for button batteries in the esophagus, and endoscopy within 6 hours for multiple magnets in any gastrointestinal location (21). In our study, 98.2% (122/124) of high-risk foreign bodies were removed within the guideline-recommended time, with a severe complication rate (perforation/mediastinitis) of 4.8%, which was lower than the international reported rate (10–15%), indicating that timely intervention in accordance with guidelines can effectively reduce severe complications. However, in a 2024 survey on pediatric endoscopy training initiated by 58 medical centers across 12 countries by APSPGHAN, it was found that: only 36% of the study programs employed competency-based outcomes for program development, whereas nearly half (48%) used volume-based curricula, the direct observation of procedural skills was the most commonly used assessment method (22). High-risk foreign bodies in children not only require primary physicians to have precise identification and risk assessment capabilities, but also pose higher challenges to the skills of operators performing foreign body removal. Therefore, it is recommended to enhance standardized training for foreign body removal procedures via gastric endoscopy in pediatric regional centers to cultivate medical talents who can better handle clinical situations.
Magnetic digestive foreign bodies also belong to high-risk foreign bodies. When they adhere to each other at different sites within the gastrointestinal tract, the perforation rate can be as high as 50% to 75% (23). A national survey showed that ingestion of multiple magnetic foreign bodies requires more invasive treatment than ingestion of a single one (24). In this survey, there were 78 cases of magnetic bead foreign bodies, among them, 7 cases had multiple magnetic beads (≥2 beads) (all classified as high-risk foreign bodies), and 71 cases had a single magnetic bead (classified as medium-risk foreign body). Among the 7 cases with multiple magnetic beads, 2 cases had perforation, 3 cases had ulcers, and 2 cases had esophagitis/gastritis. The complication rate reached 100%, which was significantly higher than 5.6% (4/71) in the cases with a single magnetic bead. This further confirmed the high-risk characteristic that multiple magnetic foreign bodies easily cause digestive tract damage due to their mutual adhesion. The “Expert Consensus on Endoscopic Management of Foreign Bodies in the Upper Gastrointestinal Tract of China” suggests that multiple magnetic foreign bodies should undergo emergency endoscopy, and even a single magnetic foreign body should be removed via elective endoscopy (25,26). Multiple studies have shown that after accidental ingestion of magnetic foreign bodies, most children initially present with mild or no clinical symptoms for the first few hours or weeks, followed by the gradual onset of persistent or intermittent abdominal pain, nausea, vomiting, and other symptoms (27-29). Therefore, timely diagnosis and effective management of ingestion of multiple magnetic foreign bodies or a single magnetic foreign body along with a metallic foreign body are crucial for reducing the occurrence of complications.
In addition, comorbid mental disorders were identified as a high-risk factor for complications from GIFB in the results (P=0.006, OR =3.780, 95% CI: 1.450–9.860). In this study, there were 35 older children (over 12 years old), and the primary cause of GIFB in this group was intentional swallowing. Among them, one case involved a female child with repeated ingestion of hair, a behavior often associated with the psychiatric condition trichophagia. Literature reviews indicate that trichophagia occurs predominantly in females, and without psychological intervention, it is prone to recurrence (30). Follow-up on children with GIFB revealed that a significant proportion had comorbid mental or psychological disorders, with some experiencing repeated hospitalizations. Therefore, for older children who intentionally swallow foreign bodies, after managing the GIFB, psychological counseling and treatment are also necessary. Parents and healthcare providers should prioritize psychological guidance to help these children address their mental health issues, as this is a key measure to prevent recurrent ingestion of foreign bodies.
Limitations
This study has several specific limitations related to regional clinical practice: (I) the endoscopy intervention rate (72.3%) in our center is significantly higher than that in Western studies (10–20%), which is attributed to three factors: high parental vigilance for pediatric GIFB in China, the characteristics of severe cases in tertiary referral centers, and domestic clinical guidelines advocating active endoscopic intervention to prevent severe complications; (II) as a single-center study in eastern China, the results may not be directly generalized to rural areas or other regions with different healthcare access; (III) the retrospective design may lead to potential recall bias of retention time by caregivers.
Interpretation
Our findings are biologically plausible. Younger children’s smaller gastrointestinal lumens and immature swallowing coordination increase risk. Upper esophageal retention poses greater danger due to anatomical narrowness. Prolonged retention causes progressive mucosal damage. Intentional swallowing and mental disorders likely reflect behavioral issues leading to delayed presentation. The higher complication rate compared to Western studies may reflect healthcare access disparities rather than true population differences. Caution is needed in extrapolating these risk estimates to primary care settings where milder cases predominate.
Generalisability
These results are generalizable to similar tertiary pediatric emergency settings in urban China and other middle-income countries with comparable healthcare systems and foreign body epidemiology. The regional high-risk early warning criterion for pediatric GIFB (age <4 years + upper esophagus retention + retention time >24 h) provides a practical clinical tool for emergency physicians. However, application to rural settings or countries with different foreign body types and healthcare access patterns requires validation. Our findings support region-specific prevention strategies and emergency protocols.
Conclusions
This study retrospectively analyzed 726 cases of foreign body digestion in children in our hospital from 2021 to 2024, aiming to explore their clinical characteristics, the occurrence of complications and related risk factors. By identifying high-risk groups and risk factors, it not only provides a reference for the early intervention of emergency doctors, but also is of great significance for the prevention and health education of children accidentally swallowing foreign objects. It reveals the common types of foreign bodies in the digestive tract among children and the occurrence of their complications, emphasizing the importance of paying attention to high-risk groups and timely treatment. The research results provide an important basis for future clinical practice and have practical application value for improving pediatric emergency rescue and preventive measures. Future research should continue to explore prevention and management strategies for foreign bodies in the digestive tract to reduce their impact on children’s health. Further research can provide a scientific basis for formulating more effective intervention measures and family guidance. At present, there are many retrospective studies on gastrointestinal foreign bodies in children abroad, but most of them are single-center or have limited sample sizes. The research results vary greatly among different regions. In China, especially in regions, large-scale systematic analyses of large samples are still relatively insufficient, and the clinical understanding of risk factors for complications is not yet unified. Therefore, summarizing large-scale case data is helpful to fill the research gap.
Acknowledgments
The authors thank the emergency department and endoscopy unit staff of Children’s Hospital, Zhejiang University School of Medicine for their assistance in data collection and patient care. We also acknowledge the contribution of the medical records department for facilitating access to electronic medical records.
Footnote
Reporting Checklist: The authors have completed the STROBE reporting checklist. Available at https://tp.amegroups.com/article/view/10.21037/tp-2026-1-0009/rc
Data Sharing Statement: Available at https://tp.amegroups.com/article/view/10.21037/tp-2026-1-0009/dss
Peer Review File: Available at https://tp.amegroups.com/article/view/10.21037/tp-2026-1-0009/prf
Funding: This research work was supported by
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://tp.amegroups.com/article/view/10.21037/tp-2026-1-0009/coif). The authors have no conflicts of interest to declare.
Ethical Statement: The study was conducted in accordance with the Declaration of Helsinki and its subsequent amendments. The study was approved by Medical Ethics Committee of the Children’s Hospital, Zhejiang University School of Medicine (No. 2025-IRB-0115-P-01) and individual consent for this analysis was waived due to the retrospective nature.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Chinese Medical Association Pediatric Endoscopy Collaboration Group, Chinese Medical Doctor Association Pediatric Digestive Endoscopy Committee. Management of foreign bodies in the digestive tract of children in China: a clinical practice guideline (2021). Chinese Journal of Evidence-Based Medicine 2022;22:2-18.
- Chinese Medical Association Pediatric Digestive Group, Editorial Board of Chinese Journal of Pediatrics. Expert consensus on diagnosis, management and endoscopic treatment of aerodigestive tract foreign bodies in Chinese children. Chin J Pediatr 2022;60:401-7. [Crossref] [PubMed]
- Rybojad B, Niedzielska G, Niedzielski A, et al. Esophageal foreign bodies in pediatric patients: a thirteen-year retrospective study. ScientificWorldJournal 2012;2012:102642. [Crossref] [PubMed]
- Protocolo Clínico E, de Regulação Ingestão, de Corpo Estranho. Secretaria de Estado da Saúde do Estado do Espírito Santo-SESA: 2023. Available online: https://saude.es.gov.br/Media/sesa/Protocolo/Protocolo_Cl%C3%ADnico_e_de_Regula%C3%A7%C3%A3o_em_Ingest%C3%A3o_de_Corpo_Estranho.pdf
- Karišik M. Foreign body aspiration and ingestion in children. Acta Clin Croat 2023;62:105-12. [Crossref] [PubMed]
- Demiroren K. Management of Gastrointestinal Foreign Bodies with Brief Review of the Guidelines. Pediatr Gastroenterol Hepatol Nutr 2023;26:1-14. [Crossref] [PubMed]
- Gu ZJ, Liu HF, Cheng WW, et al. Risk factors for severe complications caused by digestive tract foreign bodies in children. Journal of Clinical Pediatrics 2018;36:734-7.
- Li ML, Chen MM, Huang XP, et al. Analysis on ingested foreign bodies in children and the intervention: 171 cases. Journal of Guangdong Medical University 2019;37:321-4.
- Chen J, Duan JT, Yang LH, et al. Clinical characteristics of 200 children with foreign bodies in the digestive tract and analysis in risk factors of complications. Journal of Clinical Medicine in Practice 2021;25:72-5.
- Isa HM, Aldoseri SA, Abduljabbar AS, et al. Accidental ingestion of foreign bodies/harmful materials in children from Bahrain: A retrospective cohort study. World J Clin Pediatr 2023;12:205-19. [Crossref] [PubMed]
- Fang GC, Huang KY. Retrospective analysis of 756 cases of ingested foreign bodies in the upper gastrointestinal tract in children treated with electronic endoscopy. Chinese Journal of Practical Pediatrics 2023;38:775-8.
- Chen YT. Analysis of Clinical Characteristics and Risk Factors of 180 Cases of Pediatric Gastrointestinal Foreign Bodies in Fuzhou Area. Guide of China Medicine 2023;21:40-2,47.
- Du M, Shang LH, Xiang M, et al. Clinical features, risk factors for complications, and treatment methods of 980 children with foreign bodies in the digestive tract. Shandong Medical Journal 2020;60:60-2.
- Orsagh-Yentis D, McAdams RJ, Roberts KJ, et al. Foreign-Body Ingestions of Young Children Treated in US Emergency Departments: 1995-2015. Pediatrics 2019;143:e20181988. [Crossref] [PubMed]
- Emeka CK, Chukwuebuka NO, Tochukwu EJ. Foreign body in the gastrointestinal tract in children: A tertiary hospital experience. Afr J Paediatr Surg 2023;20:224-8. [Crossref] [PubMed]
- Chen Y, Zhuo L, Kong XX, et al. Analyzing the risk factors of upper gastrointestinal tract injury caused by foreign bodies. Journal of Clinical Emergency 2022;23:61-6.
- Lin CF, Lin QB, Zheng WN. Epidemiological investigation of foreign bodies in digestive tract and analysis of influencing factors of complications in the last 10 years. China Journal of Endoscopy 2023;29:49-56.
- Ren L, Geng LL, Xiao WQ, et al. A systemic report of 1 257 cases of ingested foreign bodies in children. Chinese Journal of Evidence-Based Pediatrics 2017;12:333-6.
- Speidel AJ, Wölfle L, Mayer B, et al. Increase in foreign body and harmful substance ingestion and associated complications in children: a retrospective study of 1199 cases from 2005 to 2017. BMC Pediatr 2020;20:560. [Crossref] [PubMed]
- Li YW, Wang YS, Zhou XH. Clinical analysis of 260 cases of pediatric upper gastrointestinal foreign bodies treated by gastroscopy. Chinese General Practice Nursing 2024;22:1516-8.
- Tringali A, Thomson M, Dumonceau JM, et al. Pediatric gastrointestinal endoscopy: European Society of Gastrointestinal Endoscopy (ESGE) and European Society for Paediatric Gastroenterology Hepatology and Nutrition (ESPGHAN) Guideline Executive summary. Endoscopy 2017;49:83-91. [Crossref] [PubMed]
- Ukarapol N, Tanatip N, Sharma A, et al. Current Pediatric Endoscopy Training Situation in the Asia-Pacific Region: A Collaborative Survey by the Asian Pan-Pacific Society for Pediatric Gastroenterology, Hepatology and Nutrition Endoscopy Scientific Subcommittee. Pediatr Gastroenterol Hepatol Nutr 2024;27:258-65. [Crossref] [PubMed]
- Miyamoto R, Okuda M, Kikuchi S, et al. A nationwide questionnaire survey on accidental magnet ingestion in children in Japan. Acta Paediatr 2021;110:314-25. [Crossref] [PubMed]
- Yu D, Yan JY, Lu HT. Literature analysis of magnetic foreign bodies in the digestive tract of Chinese children. Chinese Journal of Pediatric Surgery 2025;46:121-8.
- Ge W, Lian P, Li Y, et al. Clinical characteristics and therapeutic experience of magnetic foreign body ingestion in children. Journal of Clinical Pediatric Surgery 2021;20:1174-8.
- Chen J. Management principles of foreign bodies in digestive tract: Magnetic foreign body ingestion. Chinese Journal of Practical Pediatrics 2021;36:924-6.
- Mo YL, Hu XH, Zhang PF, et al. Diagnosis and treatment of magnetic foreign bodies in digestive tract of children: a single center 10-year study on 28 cases. Chinese Journal of Practical Medicine 2020;47:5-9.
- Zhou F, Wang RF, Zhou L, et al. Retrospective analysis of 31 cases of multiple magnetic foreign bodies ingestion in children. Journal of Clinical Pediatrics 2021;39:147-51.
- Chen D, Wei Q, Jia XJ. Clinical analysis of magnetic foreign bodies in the digestive tract of children. Maternal and Child Health Care of China 2024;39:458-61.
- Jiang GP, Ruan WW, Yuan XQ. Clinical analysis of 12 cases of trichobezoar in children. Modern Practical Medicine 2023;35:520-2.