Trends and insights in non-syndromic craniosynostosis research globally: a bibliometric analysis of the Web of Science database (2005–2024)
Highlight box
Key findings
• Global non-syndromic craniosynostosis (NSC) research output increased steadily from 2005 to 2024, with an inflection point in 2012 and stabilization after 2018.
• The United States dominates publication volume and international collaboration networks, but cross-institutional and cross-continental collaboration remains limited.
• Three foundational knowledge domains were identified: intracranial pressure physiology, endoscopic surgical innovation, and neurodevelopmental outcomes.
• Research hotspots have shifted from genetics (2005–2014) to surgical techniques (2015–2020) and, most recently, to long-term neurodevelopmental and psychosocial outcomes (2021–2024).
What is known and what is new?
• NSC is a common congenital cranial deformity with well-described surgical techniques and emerging genetic associations, but the global intellectual structure and thematic evolution of the field have never been systematically mapped.
• This study provides the first bibliometric mapping of two decades of NSC research, identifying foundational knowledge domains, citation bursts, emerging hotspots, and critical knowledge gaps – including the paucity of long-term psychosocial outcomes and the incomplete translation of genetic discoveries into clinical practice.
What is the implication, and what should change now?
• The findings highlight the need for harmonized international patient registries and a greater focus on socio-economic and psychosocial outcomes beyond traditional surgical metrics.
• Future research should prioritize interdisciplinary and international consortia to break down research silos, validate genetic biomarkers, and develop translational frameworks linking molecular discoveries with individualized clinical care.
Introduction
Non-syndromic craniosynostosis (NSC) is the most prevalent form of craniosynostosis, a congenital craniofacial anomaly characterized by the premature fusion of one or more cranial sutures (1). Early suture closure disrupts normal skull growth patterns, leading to abnormal cranial morphology and potentially altered intracranial volume (2). NSC accounts for approximately 80% of all craniosynostosis cases and differs from syndromic forms (e.g., Apert or Crouzon syndrome) in that it typically presents as an isolated defect without other systemic anomalies (3).
NSC affects an estimated 1 in 2,000 to 2,500 live births globally. The sagittal suture is most frequently involved, followed by metopic, unicoronal, and unilambdoid sutures (4,5). In addition to cranial deformities and potential elevation of intracranial pressure (ICP), affected children often exhibit neurodevelopmental challenges, including cognitive delay, language impairment, and learning disabilities (6-8). Without timely surgical intervention, NSC can lead to severe craniofacial dysmorphology and irreversible neurological consequences (9).
The etiology of NSC is multifactorial, involving complex interactions between genetic susceptibility and environmental exposures. A landmark genome-wide association study (GWAS) by Justice et al. (2012) identified several risk loci, although the incomplete penetrance of these variants suggests contributions from epigenetic and environmental modulators (10). A recent developmental study has shown that cranial sutures originate from both neural crest and mesoderm-derived stem cells, which must remain in dynamic balance to maintain suture patency and support normal skull morphogenesis. Disruption of this balance may initiate premature suture fusion (11).
Surgical correction remains the cornerstone of NSC management, with major techniques including strip craniectomy, cranial vault remodeling, and spring-mediated cranioplasty (12-14). Distraction osteogenesis has also shown promise, especially in complex or syndromic cases, though long-term outcome data remain limited (15,16). Despite these technical advances, a global consensus on the optimal timing, surgical approach, or long-term neurodevelopmental impact remains elusive, with considerable variation across institutions and regions.
While significant progress has been made in understanding the clinical and developmental aspects of NSC, major knowledge gaps persist. In particular, there is limited understanding of how NSC research has evolved across countries, institutions, and disciplines. Traditional narrative reviews, while valuable for synthesizing established knowledge, are inherently limited in their ability to quantitatively map the structure of a research field, detect emerging thematic shifts, or visualize collaborative networks that may reveal hidden silos or translational bottlenecks. Bibliometric analysis—a quantitative method for evaluating the structure, output, and trends of scientific literature—offers a powerful approach to mapping the global landscape of NSC scholarship (17).
In this study, we conducted a comprehensive bibliometric analysis of NSC-related publications from 2005 to 2024 using VOSviewer, CiteSpace, and the R-based bibliometrix package. Our objectives were to: (I) identify the most productive countries, institutions, authors, and journals; (II) characterize global collaboration patterns; and (III) map evolving research hotspots and foundational literature. These findings aim to inform future research priorities and support international collaboration in pediatric craniofacial science. We present this article in accordance with the BIBLIO reporting checklist (available at https://tp.amegroups.com/article/view/10.21037/tp-2025-1-930/rc).
Methods
Data sources and search strategy
We conducted a comprehensive literature search on 20 June 2025 using the Web of Science Core Collection (WoSCC) database (Clarivate Analytics, https://www.webofscience.com/wos/woscc/basic-search), a widely recognized bibliometric data source indexing over 34,000 journals across scientific disciplines. The search strategy employed Boolean operators and controlled vocabulary as follows: ((TS=(Nonsyndromic Craniosynostosis)) OR TS=(Non-syndromic craniosynostosis)). The search covered publications from 1 January 2005 to 31 December 2024.
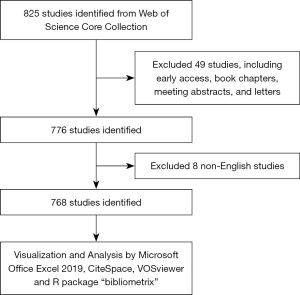
The year 2005 was selected as the starting point based on its disciplinary significance: it coincides with the widespread clinical adoption of endoscope-assisted strip craniectomy, which fundamentally shifted surgical paradigms from exclusively open approaches toward minimally invasive techniques, thereby reshaping subsequent research priorities. This temporal baseline allows the analysis to capture the full trajectory of the modern surgical era and the subsequent integration of genetic discoveries following the 2012 GWAS. Only original research articles and review articles written in English were included. We retrieved metadata for each record, including title, abstract, authors, institutional affiliations, country/region, source journal, keywords, and cited references. A PRISMA-style flow diagram (Figure 1) illustrates the literature selection process.
Inclusion and exclusion criteria
Inclusion criteria: (I) articles addressing NSC in human subjects; (II) original research or review articles indexed in WoSCC; (III) English-language publications within the defined timeframe.
Exclusion criteria: (I) articles unrelated to NSC (e.g., syndromic craniosynostosis, animal-only studies, conference abstracts); (II) editorials, letters, commentaries, and corrections; (III) non-English publications.
Bibliometric analysis tools
Three complementary bibliometric software packages were used:
- VOSviewer (version 1.6.18; Leiden University, the Netherlands) for constructing and visualizing co-authorship, co-citation, and keyword co-occurrence networks. Node size reflects the number of occurrences or citations; color indicates cluster membership; line thickness represents link strength (18,19).
- CiteSpace (version 6.1.R1; Chaomei Chen, Drexel University) for collaboration network analysis, dual-map overlays, citation burst detection, and timeline visualizations (20).
- Bibliometrix R package (version 4.1.2; https://www.bibliometrix.org) for thematic evolution analysis and mapping the global distribution of NSC publications (21).
Data visualization and clustering parameters
In VOSviewer, the minimum keyword occurrence threshold was set at 5, and the minimum number of documents per author was set at 3 for author network analysis. In CiteSpace, pruning algorithms (Pathfinder, pruning sliced networks) were applied to reduce network complexity. Cluster labels were assigned using the log-likelihood ratio (LLR) algorithm. All maps were manually inspected for accuracy and labeled for interpretability.
To enhance accessibility for the clinical readership, we provide the following interpretations of key bibliometric indicators used throughout this study:
- Citation bursts: detect articles that have received a sudden surge of citations over a specific period, indicating emerging topics or paradigm-shifting discoveries that have rapidly gained attention.
- Co-citation analysis: when two references are frequently cited together, they represent shared intellectual foundations; clustering co-cited references reveals the “knowledge base” of a field.
Data management and supplementary analyses were conducted using Microsoft Excel 2019.
Ethics
This study analyzed publicly available, non-identifiable bibliographic data and therefore did not require institutional ethics approval.
Results
Quantitative overview of publications
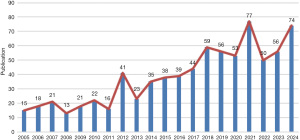
A total of 768 publications on NSC were retrieved between 2005 and 2024. As shown in Figure 2, the annual number of publications has followed a trajectory that mirrors key disciplinary milestones. The field remained relatively quiet from 2005 to 2011 (mean: 18 articles/year), but a marked inflection point occurred in 2012, coinciding with the publication of the first GWAS on NSC by Justice et al., which catalyzed renewed genetic investigations (10). A second surge occurred after 2018, with output stabilizing at a higher plateau (mean: 61 articles/year) and peaking at 77 articles in 2021. This post-2018 stability reflects the maturation of minimally invasive surgical techniques and a growing research emphasis on long-term neurocognitive outcomes rather than purely technical refinements.
Country and institutional contributions
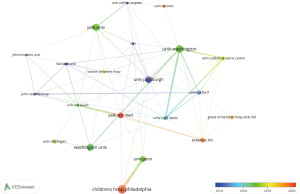
These publications originated from 56 countries and 928 institutions. The top 10 contributing countries were primarily from Europe (n=6) and North America (n=2), with the United States leading by a substantial margin (403 articles, 42.5%), followed by England (n=72), Netherlands (n=44), and Canada (n=36) (Table 1). A co-authorship network (Figure 3) constructed from countries with ≥3 publications revealed the USA’s central position in international collaboration, particularly with England, the Netherlands, Canada, and China.
Table 1
| Rank | Country | Institution | |||
|---|---|---|---|---|---|
| Name | Counts (%) | Name | Counts (%) | ||
| 1 | USA (North America) | 403 (42.5) | Children’s Hospital Philadelphia (USA) | 34 (1.74) | |
| 2 | England (Europe) | 72 (7.6) | University of Washington (USA) | 30 (1.53) | |
| 3 | Netherlands (Europe) | 44 (4.6) | Washington University (USA) | 28 (1.43) | |
| 4 | Canada (North America) | 36 (3.8) | Yale University (USA) | 28 (1.43) | |
| 5 | Italy (Europe) | 34 (3.6) | University Pittsburgh (USA) | 27 (1.38) | |
| 6 | France (Europe) | 32 (3.4) | University of Pennsylvania (USA) | 25 (1.28) | |
| 7 | Australia (Oceania) | 31 (3.3) | Yale School of Medicine (USA) | 23 (1.17) | |
| 8 | Germany (Europe) | 29 (3.1) | Erasmus Medisch Centrum (Netherlands) | 19 (0.97) | |
| 9 | Sweden (Europe) | 24 (2.5) | University of Oxford (England) | 18 (0.92) | |
| 10 | China (Asia) | 20 (2.1) | University Cattolica Sacro Cuore (Italy) | 17 (0.87) | |

Among the top 10 most productive institutions, seven were based in the USA. The leading institutions were the Children’s Hospital of Philadelphia (n=34), the University of Washington (n=30), and Washington University (n=28). A network of institutions with ≥10 publications (Figure 4) showed that the University of Washington had earlier research involvement but fewer publications than the Children’s Hospital of Philadelphia. Notably, no direct collaboration was observed between the top two institutions.
Journal and co-cited journal analysis
NSC-related studies were published in 162 academic journals. The three most prolific outlets were Journal of Craniofacial Surgery (n=211, 27.5%), Plastic and Reconstructive Surgery (n=85, 11.1%), and Child’s Nervous System (n=67, 8.7%) (Table 2). Among the top 15 journals, the highest impact factors (IFs) were reported for Scientific Reports (IF =3.9) and Plastic and Reconstructive Surgery (IF =3.4). A co-citation map of 17 journals with ≥5 related publications (Figure 5A) revealed active citation interrelationships among the top three journals.
Table 2
| Rank | Journal | Co-cited journal | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Journal name | Count (%) | IF | Q | Journal name | Co-citation | IF | Q | ||
| 1 | Journal of Craniofacial Surgery | 211 (27.5) | 1 | 3 | Plastic and Reconstructive Surgery | 3,616 | 3.4 | 1 | |
| 2 | Plastic and Reconstructive Surgery | 85 (11.1) | 3.4 | 1 | Journal of Craniofacial Surgery | 2,738 | 1 | 3 | |
| 3 | Child’s Nervous System | 67 (8.7) | 1.2 | 3 | Child’s Nervous System | 1,533 | 1.2 | 3 | |
| 4 | Journal of Neurosurgery: Pediatrics | 60 (7.8) | 2.1 | 2 | Journal of Neurosurgery: Pediatrics | 940 | 2.1 | 2 | |
| 5 | Cleft Palate-Craniofacial Journal | 37 (4.8) | 1.3 | 3 | Journal of Neurosurgery | 918 | 2.1 | 2 | |
| 6 | Journal of Cranio-Maxillo-Facial Surgery | 21 (2.7) | 2.1 | 2 | Cleft Palate-Craniofacial Journal | 635 | 3.6 | 1 | |
| 7 | American Journal of Medical Genetics, Part A | 19 (2.5) | 1.7 | 3 | American Journal of Medical Genetics, Part A | 588 | 1.7 | 3 | |
| 8 | Annals of Plastic Surgery | 12 (1.6) | 1.6 | 2 | Nature Genetics | 454 | 29 | 2 | |
| 9 | Pediatric Neurosurgery | 8 (1.0) | 1.3 | 3 | Pediatrics | 418 | 6.4 | 1 | |
| 10 | Neurosurgical Focus | 7 (0.9) | 3 | 1 | American Journal of Human Genetics | 363 | 8.1 | 1 | |
| 11 | Scientific Reports | 6 (0.8) | 3.9 | 1 | Neurosurgery | 332 | 3.9 | 1 | |
| 12 | Journal of Plastic, Reconstructive and Aesthetic Surgery | 6 (0.8) | 2.4 | 1 | Journal of Cranio-Maxillo-Facial Surgery | 329 | 2.1 | 2 | |
| 13 | Plastic Surgery | 5 (0.7) | 0.6 | 4 | Pediatric Neurosurgery | 305 | 1.3 | 3 | |
| 14 | Journal of Anatomy | 5 (0.7) | 1.9 | 2 | Neurosurgical Focus | 225 | 3 | 1 | |
| 15 | Acta Neurochirurgica | 5 (0.7) | 1.9 | 2 | Annals of Plastic Surgery | 207 | 1.6 | 2 | |
IF, impact factor.

In terms of co-cited journals, Plastic and Reconstructive Surgery had the highest co-citation frequency (n=3,616), followed by Journal of Craniofacial Surgery (n=2,738) and Child’s Nervous System (n=1,533). High-impact journals, such as Nature Genetics (IF =29) and American Journal of Human Genetics (IF =8.1) also featured prominently. A co-citation network of journals with ≥80 citations (Figure 5B) illustrated strong interconnectivity among the leading journals.
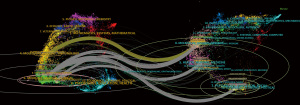
A dual-map overlay (Figure 6) showed the citation trajectories between citing and cited journals. Articles published in Molecular/Biology/Genetics clusters were frequently cited by Molecular/Biology/Immunology and Medicine/Medical/Clinical journals, while literature from Health/Nursing/Medicine and Psychology/Education/Social clusters was predominantly cited by Medicine/Medical/Clinical journals.
Author and co-cited author analysis
A total of 3,255 unique authors contributed to NSC research. The top 10 authors, each with ≥15 publications (Table 3), included Persing, John A, Taylor, Jesse A, and Bartlett, Scott P, each authoring >30 articles. A co-authorship network based on authors with ≥8 publications (Figure 7A) showed strong collaboration between Taylor and Bartlett, but not with Persing.
Table 3
| Rank | Authors | Count | Co-cited authors | Citations |
|---|---|---|---|---|
| 1 | Persing, John A | 40 | Jimenez, DF | 290 |
| 2 | Taylor, Jesse A | 34 | Fearon, JA | 255 |
| 3 | Bartlett, Scott P | 33 | Lajeunie, E | 253 |
| 4 | Alperovich, Michael | 21 | Renier, D | 214 |
| 5 | Swanson, Jordan W | 20 | Wilkie, AOM | 196 |
| 6 | Patel, Kamlesh B | 18 | Speltz, ML | 195 |
| 7 | Buchman, Steven R | 17 | Kapp-simon, KA | 191 |
| 8 | Skolnick, Gary B | 16 | Mccarthy, JG | 153 |
| 9 | Boyadjiev, Simeon A | 15 | Cohen, MM | 135 |
| 10 | Johnson, David | 15 | Di rocco, F | 135 |

Among 8,858 co-cited authors, the top three were Jimenez, D.F. (n=290), Fearon, J.A. (n=255), and Lajeunie, E. (n=253). The co-citation network (Figure 7B) for authors with ≥50 citations revealed dense collaborative clusters, especially among Jimenez and his frequent co-citees.
Co-cited references and citation bursts
A total of 12,021 references were co-cited in the NSC literature. The top 10 most frequently co-cited articles (Table 4) were each cited ≥60 times, with Renier D (1982, J Neurosurg), Magge SN (2002, J Craniofac Surg), and Kapp-Simon KA (2007, Child Nerv Syst) exhibiting high mutual co-citation (Figure 8).
Table 4
| Rank | Co-cited reference | Citations |
|---|---|---|
| 1 | Renier D, 1982, J Neurosurg, V57, P370 | 80 |
| 2 | Magge SN, 2002, J Craniofac Surg, V13, P99 | 75 |
| 3 | Kapp-Simon KA, 2007, Child Nerv Syst, V23, P269 | 75 |
| 4 | Lbecker DB, 2005, Plast Reconstr Surg, V116, P400 | 74 |
| 5 | Boulet SL, 2008, Am J Med Genet A, V146a, P984 | 74 |
| 6 | Jimenez DF, 1998, J Neurosurg, V88, P77 | 67 |
| 7 | Di Rocco F, 2009, J Neurosurg-Pediatr, V4, P21 | 65 |
| 8 | Ajeunie E, 1995, Am J Med Genet, V55, P500 | 64 |
| 9 | Kapp-Simon KA, 1998, Cleft Palate-Cran J, V35, P197 | 61 |
| 10 | Speltz ML, 2004, J Pediatr Psychol, V29, P651 | 61 |

Citation burst analysis identified 10 references with significant citation surges over defined periods (Figure 9). The most intense citation burst (strength =10.88) was for “An epidemiological study of nonsyndromal craniosynostoses” by Kolar JC, active from 2012 to 2016. The second-highest burst (strength =10.48) was observed for Shah MN’s 2014–2016 publication comparing endoscopic versus open sagittal synostosis repair. Overall, burst durations ranged from 3 to 5 years, with strengths from 7.38 to 10.88. Table 5 summarizes the core contributions of these 13 highly cited articles.

Table 5
| Rank | Strength | Main research content |
|---|---|---|
| 1 | 10.88 | An epidemiological study of nonsyndromal craniosynostoses |
| 2 | 7.6 | Prevalence and complications of single-gene and chromosomal disorders in craniosynostosis |
| 3 | 7.38 | Long-term outcomes of primary craniofacial reconstruction for craniosynostosis: a 12-year experience |
| 4 | 10.48 | Endoscopically assisted versus open repair of sagittal craniosynostosis: the St. Louis Children’s Hospital experience |
| 5 | 9.73 | The effects of whole-vault cranioplasty versus strip craniectomy on long-term neuropsychological outcomes in sagittal craniosynostosis |
| 6 | 9.3 | An evaluation of complications, revisions, and long-term aesthetic outcomes in nonsyndromic metopic craniosynostosis |
| 7 | 9.3 | The impact of age at surgery on long-term neuropsychological outcomes in sagittal craniosynostosis |
| 8 | 10.23 | A genetic-pathophysiological framework for craniosynostosis |
| 9 | 7.82 | The preoperative incidence of raised intracranial pressure in nonsyndromic sagittal craniosynostosis is underestimated in the literature |
| 10 | 9.73 | Two locus inheritance of non-syndromic midline craniosynostosis via rare and common alleles |
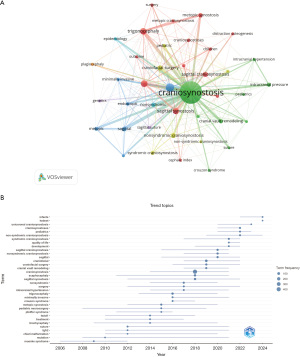
Keyword analysis and research trends
Keyword co-occurrence analysis revealed 20 high-frequency terms (Table 6). Seven distinct clusters were identified (Figure 10A):
- Cluster 1: cephalic index, children, craniosynostoses, etc.;
- Cluster 2: cranial vault remodeling, craniosynostosis, Crouzon syndrome, etc.;
- Cluster 3: coronal, craniofacial, endoscopic, etc.;
- Cluster 4: computed tomography, craniofacial surgery, non-syndromic craniosynostosis, etc.;
- Cluster 5: genetics, sagittal suture;
- Cluster 6: epidemiology, nonsyndromic;
- Cluster 7: plagiocephaly.
Table 6
| Rank | Keywords | Counts |
|---|---|---|
| 1 | Craniosynostosis | 408 |
| 2 | Craniofacial | 67 |
| 3 | Scaphocephaly | 46 |
| 4 | Trigonocephaly | 43 |
| 5 | Sagittal synostosis | 39 |
| 6 | Sagittal craniosynostosis | 29 |
| 7 | Nonsyndromic craniosynostosis | 28 |
| 8 | Craniofacial surgery | 27 |
| 9 | Sagittal | 25 |
| 10 | Metopic synostosis | 23 |
| 11 | Cranial vault remodeling | 20 |
| 12 | Nonsyndromic | 20 |
| 13 | Intracranial pressure | 19 |
| 14 | Metopic | 17 |
| 15 | Syndromic craniosynostosis | 17 |
| 16 | Endoscopic | 15 |
| 17 | Pediatric | 15 |
| 18 | Craniosynostoses | 15 |
| 19 | Epidemiology | 14 |
| 20 | Children | 14 |
Temporal analysis (Figure 10B) revealed shifting research focus over time. From 2005 to 2014, the emphasis was on genetic underpinnings (mutation, FGFR2, TWIST1). Between 2015 and 2020, attention moved toward pathophysiology and surgical techniques (minimally invasive, intracranial hypertension, cranial vault remodeling). Since 2021, research has increasingly centered on long-term outcomes, including quality of life and neurodevelopment.
Discussion
Over the past two decades, NSC research has exhibited a marked increase in academic output, reflecting growing clinical and scientific interest. From 2005 to 2011, the field was relatively underexplored, with an average of 18 publications per year. However, this changed in 2012 with a notable surge in publication volume, which rose to an average of 37 annually through 2017. Since 2018, output has stabilized at a higher level (mean =61), peaking at 77 articles in 2021 and 74 in 2024, indicating that NSC research has entered a mature phase of sustained productivity. Geographically, the United States and England have been the most prolific contributors, often engaging in collaborative efforts with the Netherlands and Canada. Nevertheless, some highly productive institutions, such as the Children’s Hospital of Philadelphia, have demonstrated limited external collaboration beyond their affiliated networks, which may hinder broader cross-institutional innovation.
These trends underscore both the expanding recognition of NSC’s clinical relevance and the need for coordinated international research frameworks. This bibliometric study sought to systematically map the evolution, intellectual foundations, and emerging directions of NSC research through co-citation analysis, keyword clustering, and thematic synthesis. By identifying key contributors, highly cited works, and future priorities, our findings provide a consolidated view of how the field has matured and where its most impactful contributions are headed.
Knowledge base
Highly co-cited references in bibliometric studies often represent the foundational knowledge and prevailing consensus of a scientific field. In the context of NSC, our analysis identified the top 10 most frequently co-cited articles that collectively delineate the intellectual framework guiding the field. Among these, the seminal work by Renier et al. (1982) remains the most cited, having established elevated ICP as a physiological marker informing surgical decision-making beyond morphological abnormalities (22). Two other pivotal contributions from Renier’s group highlighted the genetic underpinnings of coronal synostosis and the epidemiological surge in trigonocephaly (23,24). Jimenez and Barone’s introduction of endoscopy-assisted techniques marked a transformative advance in surgical practice (25). Additionally, the longitudinal research by Kapp-Simon and Speltz elucidated the neuropsychological trajectory of children with NSC, reinforcing the necessity for long-term follow-up (26-28). Studies by Magge, Becker, and Boulet contributed critical insights into developmental impairment, multidimensional outcome frameworks, and perinatal risk factors, respectively (29-31). These references converge around three intellectual domains: (I) genetic and physiological mechanisms; (II) surgical innovations; and (III) neurodevelopmental outcomes—each of which continues to shape current research and clinical practice.
Hotspots and emerging frontiers
Citation burst and keyword trend analyses revealed three emerging pillars in NSC research: (I) genetics and pathophysiology; (II) surgical management and innovation; and (III) long-term neurodevelopmental prognosis. These domains were reinforced through temporal keyword clustering, indicating thematic continuity and expanding depth over time. High-frequency keywords, such as “sagittal synostosis”, “unicoronal craniosynostosis”, and “trigonocephaly” underscore increasing interest in phenotypic subtypes and their diagnostic, prognostic, and surgical implications. A notable surge in metopic synostosis across the US and Europe, particularly among males, suggests a subtype-specific epidemiological shift potentially linked to environmental or epigenetic factors (32-34). Advances in understanding polygenic and epigenetic contributors—including BMP2-SMAD6 axis involvement—reflect growing attention to developmental mechanisms (10,35). Concurrently, a shift toward minimally invasive and individualized surgical strategies, informed by cognitive development and long-term quality of life, is reshaping the therapeutic paradigm (36,37). The rising incidence of metopic cases warrants further investigation into its etiology, emphasizing the need for granular epidemiological tracking and integrative mechanistic modeling. Collectively, NSC research is trending toward a multidisciplinary framework that integrates molecular, surgical, and neurocognitive domains.
International disparities and research silos
The substantial dominance of the United States in NSC research output raises important questions about the generalizability of current knowledge. US-centric research may disproportionately reflect the healthcare infrastructure, referral patterns, and demographic compositions specific to that country, potentially shaping global “standards of care” without adequate validation in other populations. This domestic bias is particularly consequential for epidemiological findings: the rising incidence of metopic synostosis documented primarily in North American and European cohorts may not accurately represent global trends, and the risk factors identified in these populations may have limited applicability in diverse genetic and environmental contexts.
The sparse collaboration observed between top US institutions (e.g., Children’s Hospital of Philadelphia and University of Washington) and between US and non-US partners suggests the presence of research silos that may impede knowledge diffusion. Such silos can slow the translation of discoveries into practice, duplicate research efforts, and limit the cross-pollination of ideas across disciplinary and geographic boundaries. Breaking down these silos will require intentional efforts to foster international consortia, harmonize data collection standards, and create platforms for shared learning. The increasing complexity of NSC research—integrating genetics, developmental biology, surgical innovation, and neuropsychology—demands collaborative frameworks that transcend institutional and national borders.
Knowledge blank spots: what remains unexplored
Despite the progress documented in this analysis, several critical knowledge gaps persist. First, there is a notable paucity of research on long-term psychosocial outcomes, including quality of life, self-esteem, social integration, and educational attainment in adulthood. While neurodevelopmental outcomes have received increasing attention, the broader psychosocial trajectory of individuals with NSC remains largely uncharted. This gap is particularly significant given that surgical correction, even when morphologically successful, does not guarantee optimal psychosocial functioning.
Second, the drivers of the rising metopic synostosis incidence remain poorly understood. While epidemiological studies have documented this trend, the underlying mechanisms—whether environmental exposures, epigenetic modifications, or gene-environment interactions—have not been systematically investigated. The BMP2-SMAD6 axis offers a promising molecular framework, but its potential interaction with environmental factors such as maternal thyroid dysfunction or valproate exposure requires rigorous exploration.
Third, the translation of genetic discoveries into clinical practice remains incomplete. Despite the identification of risk loci such as SMAD6 and TCF12, NSC lacks the molecular stratification that could guide individualized prognosis or surgical timing. The field has not yet integrated genomic information into clinical decision-making, representing a translational gap between basic science and patient care.
Fourth, health disparities and access to care have received minimal attention. The geographic concentration of research output in high-income countries obscures the reality that children with NSC in low- and middle-income countries face substantially different challenges in accessing timely surgical care. The absence of research on these disparities perpetuates inequities and limits the global relevance of current evidence.
Epidemiology and subtypes
NSC affects approximately 5.2 per 10,000 live births globally, with single-suture variants comprising the majority of cases (38). A 2019 estimate reported that among 84,665 children with craniosynostosis, over 70,000 were nonsyndromic (38). Significant geographic variability exists, confounded by differences in registry quality and diagnostic criteria. Among subtypes, sagittal synostosis remains the most prevalent, typically presenting with dolichocephaly and biparietal narrowing (39,40), while metopic synostosis—characterized by trigonocephaly and hypotelorism—has shown a disproportionate increase in prevalence (41-43). This trend, corroborated by European and North American studies, may reflect genuine epidemiological shifts rather than diagnostic inflation (32,33). Sex-specific distributions are also evident, with sagittal synostosis showing male predominance (≈4:1), and unilateral coronal synostosis demonstrating a female bias (≈2:3) (34). These findings point to a complex interplay of genetic, environmental, and possibly hormonal factors. Standardized diagnostic criteria and globally harmonized surveillance systems are necessary to accurately assess trends and guide targeted interventions.
Genetics and pathophysiology
NSC is increasingly recognized as a polygenic and multifactorial disorder arising from the intersection of genetic predispositions, epigenetic modifications, and mechanical influences during development (1,44). Unlike syndromic forms, NSC does not follow Mendelian inheritance, though variants in genes such as SMAD6, TCF12, and FGFR2 have been implicated (45-48). Of particular note, SMAD6 variants disrupt BMP signaling—a pathway crucial to suture patency—and may interact with common risk alleles near BMP2 (49). Dysregulation at the cellular level includes aberrant neural crest migration, osteoblast overactivity, and osteoclast insufficiency, all of which contribute to premature suture fusion (50-52). Environmental contributors such as maternal smoking, thyroid dysfunction, and exposure to valproate further compound risk, likely through epigenetic modulation (53,54). Mechanical factors, including multiple gestation and intrauterine constraint, may also suppress key inhibitory regulators like NOGGIN and IHH (55,56). Single-cell transcriptomics is now uncovering mesenchymal cell heterogeneity within sutures, offering new avenues for molecular stratification and potential therapeutic targeting (50,57). This body of evidence supports a model of NSC as a spectrum of biologically distinct entities, with implications for both diagnosis and individualized management.
Treatment and prognosis
Surgical correction remains the cornerstone of NSC management, aiming to restore cranial morphology, alleviate intracranial hypertension, and optimize neurodevelopment. Traditional open approaches, such as strip craniectomy and fronto-orbital advancement, are effective for older infants but are associated with greater morbidity (58-60). Minimally invasive, endoscopy-assisted suturectomies performed in early infancy have demonstrated equivalent morphological outcomes with reduced complications and improved cognitive metrics. This is especially true when combined with postoperative helmet therapy (61-64). Innovations such as spring-mediated cranioplasty and posterior vault distraction osteogenesis (PVDO) offer promising alternatives in select cases (65-67). Increasingly, research focuses on the long-term cognitive and behavioral outcomes of surgical intervention. Early surgery, particularly for metopic and coronal synostoses, is associated with improved executive function and academic performance (68-70). However, residual neurodevelopmental deficits remain in a subset of patients, suggesting a need for longitudinal neuropsychological follow-up and individualized educational support (71-73). A shift toward outcome-driven, multidisciplinary management models underscores the importance of registry-based surveillance and equity-focused access to care.
Strengths and limitations
This study provides the first comprehensive bibliometric overview of global NSC research, utilizing robust analytical tools and a systematic search strategy to map two decades of scholarly output. Its limitations include reliance on a single database (WoS), which may exclude relevant publications, and the inclusion of only English-language articles, potentially introducing language bias. Additionally, bibliometric methods quantify productivity and impact but cannot assess the intrinsic quality of individual studies.
Conclusions
This bibliometric analysis provides the first systematic mapping of two decades of global NSC research, revealing a field in transition from descriptive morphology toward integrated molecular, surgical, and neurocognitive science. Three dominant research axes emerged: the elucidation of genetic and epigenetic mechanisms underlying suture fusion, innovation in surgical techniques and timing, and an increasing focus on long-term neurodevelopmental and psychosocial outcomes.
Despite substantial progress, critical gaps persist. International research remains disproportionately concentrated in high-income countries, particularly the United States, raising concerns about the generalizability of current evidence to diverse populations. Collaborative silos between leading institutions limit knowledge diffusion and may slow the translation of discoveries into practice. Furthermore, the drivers of rising metopic synostosis incidence remain unexplored, and the integration of genetic findings into clinical decision-making has yet to be realized.
To accelerate progress and ensure equitable impact, we propose the following actionable priorities:
- Establish harmonized, multi-national patient registries with standardized data elements to enable robust epidemiological surveillance, comparative effectiveness research, and long-term outcome tracking across diverse populations;
- Prioritize research on socio-economic and psychosocial outcomes, including quality of life, educational attainment, and healthcare access disparities, to complement the existing focus on surgical and neurodevelopmental metrics;
- Develop translational frameworks that bridge molecular discoveries and clinical application, integrating genomic stratification into prognostic assessment and surgical timing decisions.
- Foster interdisciplinary and international consortia that transcend institutional silos, bringing together neurosurgeons, geneticists, developmental biologists, and public health researchers to address complex questions that no single discipline can solve alone.
Through these coordinated efforts, the field can advance toward precision diagnostics, risk-adapted intervention, and ultimately, equitable long-term outcomes for all children with NSC, regardless of geography or socioeconomic circumstance.
Acknowledgments
None.
Footnote
Reporting Checklist: The authors have completed the BIBLIO reporting checklist. Available at https://tp.amegroups.com/article/view/10.21037/tp-2025-1-930/rc
Peer Review File: Available at https://tp.amegroups.com/article/view/10.21037/tp-2025-1-930/prf
Funding: None.
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://tp.amegroups.com/article/view/10.21037/tp-2025-1-930/coif). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Michael A, Cristiano T, Linda CM, et al. Nonsyndromic craniosynostosis. Nat Rev Dis Primers 2025;11:12.
- Doro D, Liu A, Grigoriadis AE, et al. The Osteogenic Potential of the Neural Crest Lineage May Contribute to Craniosynostosis. Mol Syndromol 2019;10:48-57. [Crossref] [PubMed]
- Flores-Sarnat L. New insights into craniosynostosis. Semin Pediatr Neurol 2002;9:274-91. [Crossref] [PubMed]
- Kolar JC. An epidemiological study of nonsyndromal craniosynostoses. J Craniofac Surg 2011;22:47-9. [Crossref] [PubMed]
- Kim DK, Green TC, Ascherman JA. Leveraging novel diagnostic codes for craniosynostosis by suture type in surgical database research. J Plast Reconstr Aesthet Surg 2025;108:18-21. [Crossref] [PubMed]
- Panchal J, Amirsheybani H, Gurwitch R, et al. Neurodevelopment in children with single-suture craniosynostosis and plagiocephaly without synostosis. Plast Reconstr Surg 2001;108:1492-8; discussion 1499-500. [Crossref] [PubMed]
- Ihnat J, Hu KG, Goss J, et al. Long-term neurocognitive and behavioral outcomes in patients with non-syndromic craniosynostosis. Childs Nerv Syst 2025;41:233. [Crossref] [PubMed]
- Collett BR, Kapp-Simon KA, Wallace E, et al. Attention and executive function in children with and without single-suture craniosynostosis. Child Neuropsychol 2017;23:83-98. [Crossref] [PubMed]
- Junn AH, Long AS, Hauc SC, et al. Long-term neurocognitive outcomes in 204 single-suture craniosynostosis patients. Childs Nerv Syst 2023;39:1921-8. [Crossref] [PubMed]
- Justice CM, Yagnik G, Kim Y, et al. A genome-wide association study identifies susceptibility loci for nonsyndromic sagittal craniosynostosis near BMP2 and within BBS9. Nat Genet 2012;44:1360-4. [Crossref] [PubMed]
- Bok S, Yallowitz AR, Sun J, et al. A multi-stem cell basis for craniosynostosis and calvarial mineralization. Nature 2023;621:804-12. [Crossref] [PubMed]
- Elawadly A, Smith L, Borghi A, et al. 3-Dimensional Morphometric Outcomes After Endoscopic Strip Craniectomy for Unicoronal Synostosis. J Craniofac Surg 2023;34:322-31. [Crossref] [PubMed]
- Bir SC, Ambekar S, Notarianni C, et al. Odilon Marc Lannelongue (1840-1911) and strip craniectomy for craniosynostosis. Neurosurg Focus 2014;36:E16. [Crossref] [PubMed]
- Rodgers W, Glass GE, Schievano S, et al. Spring-Assisted Cranioplasty for the Correction of Nonsyndromic Scaphocephaly: A Quantitative Analysis of 100 Consecutive Cases. Plast Reconstr Surg 2017;140:125-34. [Crossref] [PubMed]
- Mundinger GS, Rehim SA, Johnson O 3rd, et al. Distraction Osteogenesis for Surgical Treatment of Craniosynostosis: A Systematic Review. Plast Reconstr Surg 2016;138:657-69. [Crossref] [PubMed]
- Park DH, Yoon SH. Transsutural distraction osteogenesis for 285 children with craniosynostosis: a single-institution experience. J Neurosurg Pediatr 2016;17:230-9. [Crossref] [PubMed]
- Büttner F, Ardern CL, Blazey P, et al. Counting publications and citations is not just irrelevant: it is an incentive that subverts the impact of clinical research. Br J Sports Med 2021;55:647-8. [Crossref] [PubMed]
- van Eck NJ, Waltman L. Software survey: VOSviewer, a computer program for bibliometric mapping. Scientometrics 2010;84:523-38. [Crossref] [PubMed]
- Yang Y, Chen Y, Liu Y, et al. Mesenchymal stem cells and pulmonary fibrosis: a bibliometric and visualization analysis of literature published between 2002 and 2021. Front Pharmacol 2023;14:1136761. [Crossref] [PubMed]
- Synnestvedt MB, Chen C, Holmes JH. CiteSpace II: visualization and knowledge discovery in bibliographic databases. AMIA Annu Symp Proc 2005;2005:724-8.
- Humberto A, Edison Renato S, Marcus L, et al. VOSviewer and Bibliometrix. J Med Libr Assoc 2023;110:422-33.
- Renier D, Sainte-Rose C, Marchac D, et al. Intracranial pressure in craniostenosis. J Neurosurg 1982;57:370-7. [Crossref] [PubMed]
- Lajeunie E, Le Merrer M, Bonaïti-Pellie C, et al. Genetic study of nonsyndromic coronal craniosynostosis. Am J Med Genet 1995;55:500-4. [Crossref] [PubMed]
- Di Rocco F, Arnaud E, Renier D. Evolution in the frequency of nonsyndromic craniosynostosis. J Neurosurg Pediatr 2009;4:21-5. [Crossref] [PubMed]
- Jimenez DF, Barone CM. Endoscopic craniectomy for early surgical correction of sagittal craniosynostosis. J Neurosurg 1998;88:77-81. [Crossref] [PubMed]
- Kapp-Simon KA. Mental development and learning disorders in children with single suture craniosynostosis. Cleft Palate Craniofac J 1998;35:197-203. [Crossref] [PubMed]
- Speltz ML, Kapp-Simon KA, Cunningham M, et al. Single-suture craniosynostosis: a review of neurobehavioral research and theory. J Pediatr Psychol 2004;29:651-68. [Crossref] [PubMed]
- Kapp-Simon KA, Speltz ML, Cunningham ML, et al. Neurodevelopment of children with single suture craniosynostosis: a review. Childs Nerv Syst 2007;23:269-81. [Crossref] [PubMed]
- Magge SN, Westerveld M, Pruzinsky T, et al. Long-term neuropsychological effects of sagittal craniosynostosis on child development. J Craniofac Surg 2002;13:99-104. [Crossref] [PubMed]
- Becker DB, Petersen JD, Kane AA, et al. Speech, cognitive, and behavioral outcomes in nonsyndromic craniosynostosis. Plast Reconstr Surg 2005;116:400-7. [Crossref] [PubMed]
- Boulet SL, Rasmussen SA, Honein MA. A population-based study of craniosynostosis in metropolitan Atlanta, 1989-2003. Am J Med Genet A 2008;146A:984-91. [Crossref] [PubMed]
- Di Rocco F, Arnaud E, Meyer P, et al. Focus session on the changing “epidemiology” of craniosynostosis (comparing two quinquennia: 1985-1989 and 2003-2007) and its impact on the daily clinical practice: a review from Necker Enfants Malades. Childs Nerv Syst 2009;25:807-11. [Crossref] [PubMed]
- Gonzalez SR, Han A, Golinko MS. Shifting epidemiology of single-suture craniosynostosis and the need for a more granular ICD classification system: a national survey of members from the American Society of Pediatric Neurosurgeons (ASPN) and the American Society of Craniofacial Surgeons (ASCFS). Childs Nerv Syst 2019;35:1443-4. [Crossref] [PubMed]
- Robert FD, Laura AM, Renata SM, et al. Nonsyndromic craniosynostosis. Clin Plast Surg 2019;46:273-88.
- Timberlake AT, Choi J, Zaidi S, et al. Two locus inheritance of non-syndromic midline craniosynostosis via rare SMAD6 and common BMP2 alleles. Elife 2016;5:e20125. [Crossref] [PubMed]
- Hayek GM, Jimenez DF, Yates DM. Management of Unicoronal and Metopic Synostoses: Minimally Invasive Approaches. Oral Maxillofac Surg Clin North Am 2022;34:381-94. [Crossref] [PubMed]
- Jimenez DF, Moon HS. Endoscopic Approaches to Craniosynostosis. Atlas Oral Maxillofac Surg Clin North Am 2022;30:63-73. [Crossref] [PubMed]
- Shlobin NA, Baticulon RE, Ortega CA, et al. Global Epidemiology of Craniosynostosis: A Systematic Review and Meta-Analysis. World Neurosurg 2022;164:413-423.e3. [Crossref] [PubMed]
- Ursitti F, Fadda T, Papetti L, et al. Evaluation and management of nonsyndromic craniosynostosis. Acta Paediatr 2011;100:1185-94. [Crossref] [PubMed]
- Ramsey JA, Stevens PM, Coats B, et al. Comprehensive craniometry for sagittal synostosis. Neurosurg Focus 2025;58:E8. [Crossref] [PubMed]
- van der Meulen J. Metopic synostosis. Childs Nerv Syst 2012;28:1359-67. [Crossref] [PubMed]
- Gabrick KS, Wu RT, Singh A, et al. Radiographic Severity of Metopic Craniosynostosis Correlates with Long-Term Neurocognitive Outcomes. Plast Reconstr Surg 2020;145:1241-8. [Crossref] [PubMed]
- Sakamoto Y, Amano H, Ogihara N, et al. Geometric Morphometric Study on Distinguishing Metopic Craniosynostosis from Metopic Ridging. Plast Reconstr Surg Glob Open 2024;12:e6034. [Crossref] [PubMed]
- Bille A, Foss-Skiftesvik J, Juhler M. The current understanding of germline predisposition in non-syndromic sagittal craniosynostosis: a systematic review. Childs Nerv Syst 2023;39:689-700. [Crossref] [PubMed]
- Justice CM, Cuellar A, Bala K, et al. A genome-wide association study implicates the BMP7 locus as a risk factor for nonsyndromic metopic craniosynostosis. Hum Genet 2020;139:1077-90. [Crossref] [PubMed]
- Goovaerts S, Hoskens H, Eller RJ, et al. Joint multi-ancestry and admixed GWAS reveals the complex genetics behind human cranial vault shape. Nat Commun 2023;14:7436. [Crossref] [PubMed]
- Nicoletti P, Zafer S, Matok L, et al. Regulatory elements in SEM1-DLX5-DLX6 (7q21.3) locus contribute to genetic control of coronal nonsyndromic craniosynostosis and bone density-related traits. Genet Med Open 2024;2:101851. [Crossref] [PubMed]
- Tooze RS, Calpena E, Weber A, et al. Review of Recurrently Mutated Genes in Craniosynostosis Supports Expansion of Diagnostic Gene Panels. Genes (Basel) 2023;14:615. [Crossref] [PubMed]
- Twigg SR, Wilkie AO. A Genetic-Pathophysiological Framework for Craniosynostosis. Am J Hum Genet 2015;97:359-77. [Crossref] [PubMed]
- Holmes G, Gonzalez-Reiche AS, Saturne M, et al. Single-cell analysis identifies a key role for Hhip in murine coronal suture development. Nat Commun 2021;12:7132. [Crossref] [PubMed]
- Nieminen P, Morgan NV, Fenwick AL, et al. Inactivation of IL11 signaling causes craniosynostosis, delayed tooth eruption, and supernumerary teeth. Am J Hum Genet 2011;89:67-81. [Crossref] [PubMed]
- Kido S, Kuriwaka-Kido R, Imamura T, et al. Mechanical stress induces Interleukin-11 expression to stimulate osteoblast differentiation. Bone 2009;45:1125-32. [Crossref] [PubMed]
- Chawla R, Alden TD, Bizhanova A, et al. Squamosal Suture Craniosynostosis Due to Hyperthyroidism Caused by an Activating Thyrotropin Receptor Mutation (T632I). Thyroid 2015;25:1167-72. [Crossref] [PubMed]
- Carmichael SL, Ma C, Rasmussen SA, et al. Craniosynostosis and maternal smoking. Birth Defects Res A Clin Mol Teratol 2008;82:78-85. [Crossref] [PubMed]
- Brah TK, Thind R, Abel DE. Craniosynostosis: Clinical Presentation, Genetics, and Prenatal Diagnosis. Obstet Gynecol Surv 2020;75:636-44. [Crossref] [PubMed]
- Sanchez-Lara PA, Carmichael SL, Graham JM Jr, et al. Fetal constraint as a potential risk factor for craniosynostosis. Am J Med Genet A 2010;152A:394-400. [Crossref] [PubMed]
- Holmes G, Gonzalez-Reiche AS, Lu N, et al. Integrated Transcriptome and Network Analysis Reveals Spatiotemporal Dynamics of Calvarial Suturogenesis. Cell Rep 2020;32:107871. [Crossref] [PubMed]
- da Costa M, Pinheiro V, Borges PGLB, et al. Endoscopic Techniques in Sagittal Synostosis Correction: A Systematic Review and Meta-Analysis. Neurosurgery 2024;97:28-44. [Crossref] [PubMed]
- Greene AK, Mulliken JB, Proctor MR, et al. Primary grafting with autologous cranial particulate bone prevents osseous defects following fronto-orbital advancement. Plast Reconstr Surg 2007;120:1603-11. [Crossref] [PubMed]
- McClugage SG 3rd, Lepard JR, Ray PD, et al. Incidence of delayed intracranial hypertension in children with isolated sagittal synostosis following open calvarial vault reconstruction. Childs Nerv Syst 2020;36:545-50. [Crossref] [PubMed]
- Jimenez DF, Barone CM. Early treatment of coronal synostosis with endoscopy-assisted craniectomy and postoperative cranial orthosis therapy: 16-year experience. J Neurosurg Pediatr 2013;12:207-19. [Crossref] [PubMed]
- Jimenez DF, Barone CM. Multiple-suture nonsyndromic craniosynostosis: early and effective management using endoscopic techniques. J Neurosurg Pediatr 2010;5:223-31. [Crossref] [PubMed]
- Jimenez DF, McGinity MJ, Barone CM. Endoscopy-assisted early correction of single-suture metopic craniosynostosis: a 19-year experience. J Neurosurg Pediatr 2019;23:61-74. [Crossref] [PubMed]
- Shah MN, Kane AA, Petersen JD, et al. Endoscopically assisted versus open repair of sagittal craniosynostosis: the St. Louis Children’s Hospital experience. J Neurosurg Pediatr 2011;8:165-70. [Crossref] [PubMed]
- Shakir S, Humphries LS, Kalmar CL, et al. Hope Springs Eternal: Insights Into the Durability of Springs to Provide Long-Term Correction of the Scaphocephalic Head Shape. J Craniofac Surg 2020;31:2079-83. [Crossref] [PubMed]
- Villavisanis DF, Blum JD, Cho DY, et al. Long-term aesthetic and photogrammetric outcomes in non-syndromic unicoronal synostosis: comparison of fronto-orbital distraction osteogenesis and fronto-orbital advancement and remodeling. Childs Nerv Syst 2023;39:1283-96. [Crossref] [PubMed]
- Humphries LS, Zapatero ZD, Vu GH, et al. Ten Years of Posterior Cranial Vault Expansion by Means of Distraction Osteogenesis: An Update and Critical Evaluation. Plast Reconstr Surg 2022;150:379-91. [Crossref] [PubMed]
- Warschausky S, Angobaldo J, Kewman D, et al. Early development of infants with untreated metopic craniosynostosis. Plast Reconstr Surg 2005;115:1518-23. [Crossref] [PubMed]
- Shimoji T, Tominaga D, Shimoji K, et al. Analysis of pre- and post-operative symptoms of patients with mild trigonocephaly using several developmental and psychological tests. Childs Nerv Syst 2015;31:433-40. [Crossref] [PubMed]
- Arnaud E, Renier D, Marchac D. Prognosis for mental function in scaphocephaly. J Neurosurg 1995;83:476-9. [Crossref] [PubMed]
- Shim KW, Park EK, Kim JS, et al. Neurodevelopmental Problems in Non-Syndromic Craniosynostosis. J Korean Neurosurg Soc 2016;59:242-6. [Crossref] [PubMed]
- Kalmar CL, Lang SS, Heuer GG, et al. Neurocognitive outcomes of children with non-syndromic single-suture craniosynostosis. Childs Nerv Syst 2022;38:893-901. [Crossref] [PubMed]
- Gaillard L, Tjaberinga MC, Dremmen MHG, et al. Brain volume in infants with metopic synostosis: Less white matter volume with an accelerated growth pattern in early life. J Anat 2024;245:894-902. [Crossref] [PubMed]